Impact Factor
ISSN: 1449-1907
Int J Med Sci 2021; 18(14):3140-3149. doi:10.7150/ijms.58889 This issue Cite
Research Paper
Multidimensional Evaluation of All-Cause Mortality Risk and Survival Analysis for Hospitalized Patients with COVID-19
1. Department of Infectious Diseases, the First Affiliated Hospital of Chongqing Medical University, Chongqing, China.
2. No 1. Intensive Care Unit, Huoshenshan Hospital, Wuhan, China.
3. Department of Respiratory and Critical Care Medicine, Southwest Hospital, Third Military Medical University (Army Medical University), Chongqing, 400038, China.
4. Department of Radiology, Guanggu district, Hubei Maternal and Child Health Hospital, Wuhan, China.
5. 63650 Hospital of PLA, Malan, 841700, China.
6. College of Mathematics and Statistics, Chongqing University, Chongqing, China.
7. Department of Radiology, Huangshi Central Hospital, Affiliated Hospital of Hubei Polytechnic University, Huangshi, China.
8. Department of Radiology, Southwest Hospital, Third Military Medical University (Army Medical University), Chongqing, 400038, China.
*These authors contributed equally to this article.
Abstract
Background: Coronavirus disease 2019 (COVID-19) has caused over 3.8 million deaths globally. Up to date, the number of death in 2021 is more than that in 2020 globally. Here, we aimed to compare clinical characteristics of deceased patients and recovered patients, and analyze the risk factors of death to help reduce mortality of COVID-19.
Methods: In this retrospective study, a total of 2719 COVID-19 patients were enrolled, including 109 deceased patients and 2610 recovered patients. Medical records of all patients were collected between February 4, 2020, and April 7, 2020. Clinical characteristics, laboratory indices, treatments, and deep-learning system- assessed lung lesion volumes were analyzed. The effect of different medications on survival time of fatal cases was also investigated.
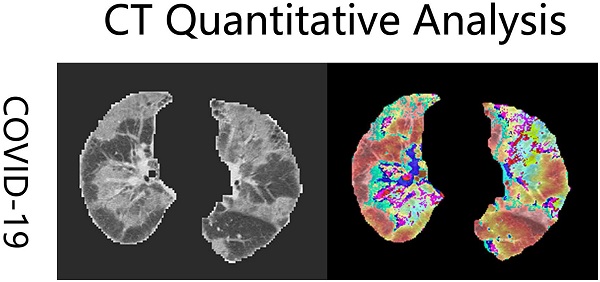
Results: The deceased patients were older (73 years versus 60 years) and had a male predominance. Nausea (10.1% versus 4.1%) and dyspnea (54.1% versus 39.2%) were more common in deceased patients. The proportion of patients with comorbidities in deceased patients was significantly higher than those in recovered patients. The median times from hospital admission to outcome in deceased patients and recovered patients were 9 days and 13 days, respectively. Patients with severe or critical COVID-19 were more frequent in deceased group. Leukocytosis (11.35×109/L versus 5.60×109/L) and lymphocytopenia (0.52×109/L versus 1.58×109/L) were shown in patients who died. The level of prothrombin time, activated partial prothrombin time, D-dimer, aspartate aminotransferase, alanine aminotransferase, urea, creatinine, creatine kinase, glucose, brain natriuretic peptide, and inflammatory indicators were significantly higher in deceased patients than in recovered patients. The volumes of ground-glass, consolidation, total lesions and total lung in all patients were quantified. Complications were more common in deceased patients than in recovered patients; respiratory failure (57.8%), septic shock (36.7%), and acute respiratory distress syndrome (26.6%) were the most common complications in patients who died. Many treatments were more frequent in deceased patients, such as antibiotic therapy (88.1% versus 53.7%), glucocorticoid treatment (70.6% versus 11.0%), intravenous immunoglobin treatment (36.6% versus 4.9%), invasive mechanical ventilation (62.3% versus 3.8%). Antivirals, antibiotics, traditional Chinese medicines and glucocorticoid treatment may significantly increase the survival time of fatal cases. Quantitative computed tomography imaging results were correlated with biochemical markers.
Conclusions: Most patients with fatal outcomes were more likely to have common comorbidities. The leading causes of death were respiratory failure and multiple organ dysfunction syndrome. Acute respiratory distress syndrome, respiratory failure and septic shock were the most common serious complications. Antivirals, antibiotics, traditional Chinese medicines, and glucocorticoid treatment may prolong the survival time of deceased patients with COVID-19.
Keywords: COVID-19, mortality risk, survival analysis

 Global reach, higher impact
Global reach, higher impact