Impact Factor
ISSN: 1449-1907
Int J Med Sci 2021; 18(12):2697-2704. doi:10.7150/ijms.59267 This issue Cite
Research Paper
The early surgical period in robotic radical hysterectomy is related to the recurrence after surgery in stage IB cervical cancer
1. Division of Gynecologic Oncology, Department of Obstetrics and Gynecology, Ajou University School of Medicine, Suwon, Republic of Korea.
2. Department of Gynecology Oncology and Robotic Surgery, Center of Hope, University of Nevada, Reno School of Medicine, Reno, NV, USA.
Abstract
Objective: To identify the pattern of recurrence and assess the clinicopathologic prognostic factors for survival after robotic radical hysterectomy (RRH) in the treatment of stage IB cervical cancer.
Methods: From December 2008 to March 2018, 64 cervical cancer patients who underwent RRH with pelvic lymph node dissection by a single surgeon were enrolled in this retrospective historical cohort timeline study. The patient's status was estimated in terms of operative outcomes, pathologic results, and survival outcomes.
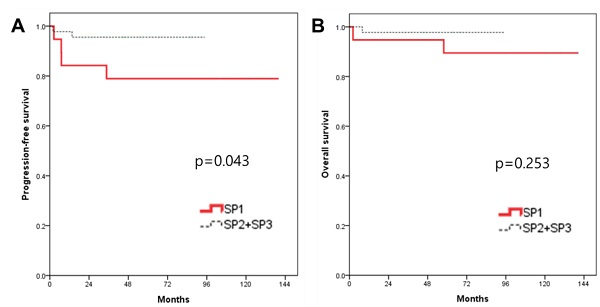
Results: The median follow-up was 63 months. The recurrence rate was 9.4% (6/64). There were two recurrences at the vaginal vault, two in the pelvic cavity, and two at the peritoneum in the intraabdominal cavity. The overall survival rate was 95.3% (61/64). When patients were divided into three groups in order based on surgery date, the first surgical period showed significantly higher recurrence rate (21%) compared to both the second (10%) and the third period (0%) (p=0.037). Multivariate analysis showed that the early period of RRH (p=0.025) and clinical tumor size more than 3 cm (p=0.003) were prognostic factors related to the recurrence. Although there was no statistical significance, there has been no recurrence since a uterine manipulator was not used.
Conclusion: The early surgical period and large tumor were related to the disease recurrence after RRH. We suggest that the achievement of proficiency and appropriate patient selection are critical for prognosis after RRH in stage IB cervical cancer.
Keywords: cervical cancer, robotic surgery

 Global reach, higher impact
Global reach, higher impact