Impact Factor ISSN: 1449-1907
Int J Med Sci 2021; 18(5):1096-1103. doi:10.7150/ijms.52433 This issue Cite
Research Paper
Microvascular Reactivity Measured by Dynamic Near-infrared Spectroscopy Following Induction of General Anesthesia in Healthy Patients: Observation of Age-related Change
1. Department of Anesthesia and Pain Medicine, Medical Research Institute, Pusan National University Hospital, Busan, Republic of Korea.
2. Department of Anesthesia and Pain Medicine, Pusan National University, School of Medicine, Yangsan, Republic of Korea
Abstract
Background: The purpose of this study was to investigate the effect of general anesthesia on microvascular reactivity and tissue oxygen saturation (StO2) using near-infrared spectroscopy in conjunction with vascular occlusion tests (VOT). Age-related changes of microvascular reactivity, that is, the capacity of capillary recruitment, were examined.
Methods: This prospective observational study was performed on 60 patients without comorbidities who underwent elective surgery under general anesthesia. Baseline StO2 on thenar eminence, hemodynamics, and laboratory profile were monitored before (T0) and 30 min after general anesthesia (T1). During VOT, occlusion slope representing oxygen consumption of muscle and recovery slope representing microvascular reactivity were also collected at T0 and T1.
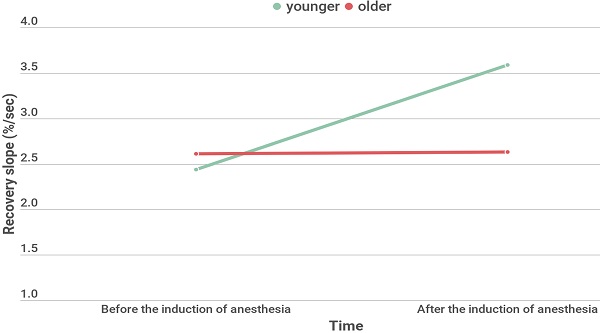
Results: Baseline StO2 and minimum / maximum StO2 during VOT increased under general anesthesia. Occlusion slope decreased while the recovery slope increased under general anesthesia. To observe aging effect, Receiver operating characteristic analysis was performed and age less than 65 years old showed a fair performance in predicting the increase of microvascular reactivity after the induction of anesthesia (AUC 0.733, 95% CI 0.594-0.845, P= 0.003). For age-related analyses, 27 patients of younger group (< 65 years) and 26 patients of older group (≥ 65 years) were divided. Recovery slope significantly increased under general anesthesia in younger group (2.44 [1.91-2.81] % ∙ sec-1 at T0 and 3.59 [2.58-3.51] % ∙ sec-1 at T1, P <0.001), but not in older group (2.61 [2.21-3.20] % ∙ sec-1 at T0, 2.63 [1.90-3.60] % ∙ sec-1 at T1, P = 0.949).
Conclusions: General anesthesia could improve StO2 through increase of microvascular reactivity and decrease of tissue metabolism. However, microvascular reactivity to capillary recruitment under general anesthesia significantly improves in younger patients, not in older patients.
Keywords: Aging, cardiovascular physiology, anesthesia, inhalation, microcirculation, spectroscopy, near-infrared

 Global reach, higher impact
Global reach, higher impact