Impact Factor ISSN: 1449-1907
Int J Med Sci 2011; 8(2):114-125. doi:10.7150/ijms.8.114 This issue Cite
Research Paper
The Influence of Hyperbaric Oxygen Treatment on the Healing of Experimental Defects Filled with Different Bone Graft Substitutes
1. Istanbul University, Faculty of Dentistry, Department of Oral Surgery, Istanbul, Turkey
2. Istanbul University, Faculty of Medicine, Department of Oncologic Pathology, Istanbul, Turkey
3. Istanbul University, Faculty of Medicine, Department of Biochemistry, Istanbul, Turkey
4. Istanbul University, Faculty of Medicine, Department of Histology and Embryology, Istanbul, Turkey.
5. Istanbul University, Faculty of Medicine, Department of Undersea and Hyperbaric Medicine, Istanbul, Turkey.
Received 2010-12-13; Accepted 2011-1-31; Published 2011-2-8
Abstract
To assess potential effects of hyperbaric oxygen (HBOT) on artificial bone grafts, β - Tricalcium phosphate (β-TCP) and calcium phosphate coated bovine bone (CPCBB) substitutes were applied to standard bone defects in rat tibiae. The control defects were left empty. Half of the animals received 60 minutes of 2.4 atmosphere absolute (ATA) of HBOT. Rats were sacrificed at one, two and four weeks. Bone healing was assessed histologically and histomorphometrically using light microscopy. The periosteum over the bone defects was examined ultrastructurally. Cardiac blood was collected to determine the serum osteocalcin levels. The HBOT increased new bone formation in the unfilled controls and β-TCP groups and significantly decreased cartilage matrix and fibrous tissue formations in all groups. Active osteoblasts and highly organized collagen fibrils were prominent in the periosteum of β-TCP and control groups. Serum osteocalcin levels also increased with HBOT. The healing of defects filled with CPCBB was similar to the controls and it did not respond to HBOT. These findings suggested that the HBOT had beneficial effects on the healing of unfilled bone defects and those filled with β-TCP bone substitute but not with CPCBB, indicating a material-specific influence pattern of HBOT.
Keywords: Hyperbaric oxygen, beta tricalcium phosphate, calcium phosphate coated bovine bone, light microscopy, ultrastuctural, rat
Introduction
Autogenous bone grafts facilitate natural healing process by providing adequate amount of mineral structure, collagen, growth factors and progenitor cells (1,2). Therefore, it is widely accepted as the "gold standard" of the bone grafting procedures in the oral and maxillofacial region. However, creation of a second surgical site, prolonged operation time, donor site morbidity, inadequate bone volume and chronic pain are also associated with clinical complications of autogenous bone harvesting (3). Thus, several alternatives to autogenous bone have been developed which use a variety of materials, including natural and synthetic polymers, ceramics, and composites (4).
β - Tricalcium phosphate (β-TCP) ceramics are bioabsorbable compounds which act as a scaffold for new vessel and bone formations (5). β-TCP has been used for alveolar bone and maxillary sinus augmentation procedures as well as the repair of periodontal and peri-implant bone defects (6,7,8). Another common bone graft used for similar clinical purposes is the particle form of inorganic bovine bone which is manufactured from animal bones. It is thermo-chemically treated in order to extract organic constituents (9). Both of these materials are potential alternatives to the autogenous bone in the osseous reconstructive surgery, especially when smaller graft volumes are required (10). However, these materials also share similar disadvantages. Long-term follow-up studies has shown significant histological delays in the replacement of these materials with newly formed bone tissue, even after six (11) and 12 months (12). Experimental studies also indicate lower overall success rate and less bone to implant contact ratio in dental implants placed in regions which were previously grafted using aforementioned types of bone substitutes (13). To overcome these issues, the fabrication of tissue engineered biomaterials, different combinations of bone grafts and systemic supportive therapy alternatives are important areas of research.
Hyperbaric oxygen therapy (HBOT) is a mode of medical treatment in which the patient breathes 100 % oxygen at a pressure greater than one atmosphere absolute (ATA) in an entirely enclosed in a pressure chamber (14). Hyperbaric condition increases the amount of oxygen dissolved in the blood; therefore, it can reach areas which are impenetrable for the red blood cells and provide tissue oxygenation in case of impaired hemoglobin concentration or function (15). In Oral and Maxillofacial surgery, HBOT is mainly used to prevent or to treat radiotherapy associated osteonecrosis of the jaws (16). In addition, this treatment modality has been found successful in increasing the incorporation rate of autogenous bone grafts (17) and soft tissue flaps (18), as well as dental implant success rates (19) in the irradiated mandible.
Although HBOT is considered a valuable adjunct on the healing of bone lesions in different anatomical regions with ischemic perfusion, the current knowledge about its influence on bone graft substitutes used in oral reconstructive surgery is limited. Therefore, the aim of this study was to evaluate histological and biochemical effects of HBOT on the healing of normally perfused experimental bone defects filled with β - TCP or calcium phosphate coated bovine bone (CPCBB) grafting materials.
Materials and Methods
Animals
The experiments were carried out on adult male Sprague-Dawley rats (N=126) weighing approximately 250 g ± 20 g, obtained from the Istanbul University, Institute for Experimental Medical Research (DETAE). All animals were housed in metallic cages in a temperature (23±10) and humidity (60-80%) controlled room under regular light and dark conditions. All procedures were reviewed and approved by the Institutional Animal Care and Use Committee at the Istanbul University, Institute for Experimental Medical Research. After several days of acclimatization, rats were randomly assigned to six experimental groups, each consisting of 21 rats. Three groups which will be breathing room air during the experiments were named as Control, B-TCP and CPCBB. The rest of the animals who will be receiving HBOT, were assigned to Control + HBOT, B-TCP + HBOT, CPCBB + HBOT groups. The HBOT was planned to be administered for one, two or four weeks. At the end of each time points, seven animals from HBOT groups were sacrificed along with an equal number of rats in non-HBOT groups. The left tibiae of the rats were used for light microscopic evaluation and right tibiae were processed for electron microscopy.
Surgical Procedures
Rats were anesthetized using intraperitoneal injection of 5 mg / kg of Xylazin hydrochloride (Rompun®, Bayer Turk Kimya San. Ltd. Sti. Istanbul, Turkey) and 60 mg / kg of Ketamin HCl (Ketanest ®, Parke Davis, Berlin, Germany). A longitudinal incision was made along the frontal aspect of both tibiae and flaps were raised to expose the bone tissue. Non-critical, four mm circular standard bone defects involving cortical and cancellous bone layers were created using a dental burr mounted on a dental rotary instrument under constant irrigation and suction. The β - TCP (Cerasorb ®,0.5-1.00 μm particle size, Curasan, Bayern, Germany) and CPCBB (Bio-Cera ®,0,6-1.00 μm particle size, Osteogenic Core Technologies, Choongnam, Korea) bone graft materials were placed using an amalgam carrier to ensure that an equal volume of each material was used for each rat. Same graft material was used in both legs. The control defects were left empty. Bleeding was controlled using sterile gauze pads. The periosteum and the skin were closed using 3.0 surgical sutures. The left tibiae of the rats were used for light microscopic evaluation and right tibiae were processed for electron microscopy.
Hyperbaric oxygen protocol
Half of the rats received HBOT in a cylindrical mono-place hyperbaric chamber. Following treatment steps were included in these sessions: 10 minutes of ventilation to fill the chamber with 100 % oxygen, five minutes of diving to 15 m (50 feet) in which the rats were exposed to 2.4 ATA pressure for 60 minutes, five minutes of re-surfacing and 10 minutes of air ventilation. The treatment started immediately after the surgical procedures were completed. The HBOT was given every day for one session at 10.00 am until the sacrification time points.
Light microscopy preparation and histomorphometric analysis
The rats were euthanized and tibiae were excised. Samples were fixated in 10 % buffered formaldehyde solution. Soft tissues were cleaned and the specimens were decalcified in formic acid sodium nitrate solution. The regions with bone defects were further sectioned and embedded in paraffin. Mid-sagittal serial sections of 7 µm thick were prepared and stained with hematoxylin and eosin. The histologic slides were examined using light microscopy under different magnifications. New bone formation (NBF), fibrous tissue formation (FTF), cartilage tissue formation (CTF) was assessed histomorphometrically using AnalySIS FIVE® digital imaging software (Olympus Soft Imaging Solutions GmBH, Münster, Germany). Sections were observed at X100 magnification and the maximum number of fields in each region that did not overlap was included. Means% ± SE% of the mean for each parameter were determined in each region.
Electron microscopy preparation
The periosteums over the bone defects were carefully dissected from the surface and the tissues were fixed in 2,5 % cacodylate buffered glutaraldehyde solution for ultra-structural examination and post-fixed in 1% osmic acid for one hour. The samples were dehydrated through a graded series of alcohol and embedded in Epon 812 (Fluka AG, Buchs Switzerland). The blocks were sectioned with LKB Ultra microtome (Stockholm, Sweden). Thick sections were stained with toluidin blue examined. Ultra thin sections selected from appropriate regions were contrasted with lead citrate and uranyl acetate and examined under and electron microscope (JEOL 1011, JEOL Ltd., Tokyo, Japan).
Serum osteocalcin measurements
1 ml of cardiac blood from the right ventricle was collected immediately after the sacrification. After the centrifugation, the serum portion was separated and processed in a rat-specific sandwich ELISA immunoassay kit (Biomedical Technologies Inc., Stoughton, U.S.A.). The amount of substrate turnover is determined colorimetrically by measuring the absorbance, which is proportional to the osteocalcin concentration.
Statistical Analysis
Graph Pad Prism® V.3 statistical analysis software (Graph Pad Software Inc., San Diego, CA, USA) was used in this study. The data was first evaluated with descriptive statistical methods such as mean and standard deviation. Kruskal-Wallis test was used for between group comparison and Dunn's multiple comparison tests was performed for subgroups. The results were evaluated in a confidence interval of 95 % and p<0.05 was considered as statistically significant.
Results
Clinical Evaluation
The animals healed uneventfully and they continued their routine physiological activities. During the experiments, two rats were lost and had to be replaced because of the complications of general anesthesia. There was no animal death related to post operative infections or HBOT procedures.
Light microscopy observations
In groups which did not receive HBOT, cartilage matrix formation was dominant both in control (Figure 1a) and in grafted defects. New bone formation was observed to start from the defect margins and extended through the center. At one week, small necrotic areas, mild inflammatory cell infiltration and scarce new vessel formation were common findings in all groups. It was found that both materials initiated foreign body reactions; however, this was more prominent for β - TCP. There were also fibrous tissue gaps between the graft particles of the same material. At two weeks, numerous new bone trabeculae were observed in the fibrous connective tissue, nearly occupying the entire defects in the control group. There was also few scattered cartilage tissue and new vessel formations. These observations were also visible around the bone grafts in the experimental defects. Nevertheless, newly formed bone was more prominent in the CPCBB groups than the β - TCP filled defects. Mild but apparent foreign body reactions were still present for both graft materials. At four weeks, all defects in the control groups were almost filled with new bone tissue in spite of the grafted sites. In β - TCP groups, the residual bone graft particles were surrounded by a combination of newly formed bone and cartilage tissue. The new bone formation in the defects of the CPCBB group was more prominent when compared to the β - TCP.
(a) Endochondral bone formation characterized by abundant cartilage matrix in the histological slide of the control group without HBOT at one week time point (H&E×100). (b) The histological slide of the control group which received HBOT at one week time point, the new bone growth and blood vessel formations (arrows) are clearly visible (H&E×250). (c) Histological appearance of the CPCBB group without HBOT at one week time point, note the arrows showing new bone trabeculae around the bone graft (H&E×40) (Cm; Cartilage matrix, Nbf; New bone formation, Gm; Graft material). (d) Light micrography of the β-TCP group without HBOT taken at two week time point (H&E ×100).
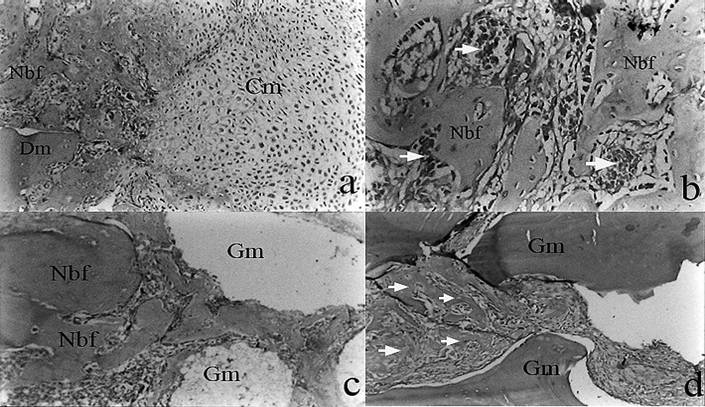
In groups which received HBOT, overall bone healing pattern was similar to non-HBO groups. However, from a subjective point of view, new bone formation was occupying larger areas which were previously filled by cartilage and fibrous connective tissues in groups which did not receive HBOT. At one week, there was no prominent inflammatory cell reaction in any of the three groups. Loose connective tissue and new bone trabeculae were found together with small islands of isolated cartilage tissue and abundant new vessels in the control group and around the bone grafts (Figure 1b, 1c). At two weeks, no cartilage or necrotic tissue formation was observed in the control group. Moreover, most of defects were already filled with newly formed bone. Similar observations were made in the groups in which the bone grafts and HBOT were used together. There were also prominent new vessel formations within the connective tissue surrounding the graft particles (Figure 1d). At four weeks, nearly all of the fibrous tissue was replaced by the newly formed bone in the control group. In β - TCP + HBOT group, there was some areas of residual graft particles surrounded mainly by a combination of mature and immature bone. Smaller areas containing graft particles were also present in CPCBB + HBOT group, however, the healing of defects in this group were close to that of the control group (Figure 2, 3 and 4).
Histomorphometry
Fibrous tissue formation: HBOT significantly reduced the amount of fibrous tissue formation at one and two week samples of the control animals, as the respective values of FTV in the Control group was calculated to be 41,4±14,2 and 29,1±9,2 whereas same values for Control + HBOT group were 25±12,1 and 14,5±4,1 (p<0.05 for both). Similarly, FTV of the CPCBB + HBOT group (23,2±10,4) was significantly lower than CPCBB group (38,4±11,9) at two weeks specimens (p< 0.05).
Cartilage matrix formation: This value was significantly lower in the control + HBOT group (48,1 ±30,5) when compared with the controls (13±11,6) (p<0.05), at one week specimens. Also, the mean CMF value in the β - TCP + HBOT group (17,1±7,8) was significantly lower than that of the β - TCP group (33±15,4) (p < 0.05) at two weeks. At the same time point, these values were respectively 9,8±4,8 for CPCBB + HBOT group and 26,4±10,6 for CPCBB group (p< 0.01) and this difference indicated a statistically significant decrease in the CMF variable in between these two groups.
New bone formation: Histomorphometric measurements revealed that the HBOT increased new bone formation in the control animals, as the NBF value in the Control + HBOT group (58,5±17,1) was significantly higher than that of the Control group (40,2±7,6) (p<0.05) at two weeks. At one and two weeks' time points, there was also an increase in the NBF value of β - TCP + HBOT (18,7±4,7 and 45,7±11, respectively) when compared to the β - TCP group (9,2±7,7 and 20,7±7,4 respectively) (p<0.05 and p< 0.01, respectively) (Table 1).
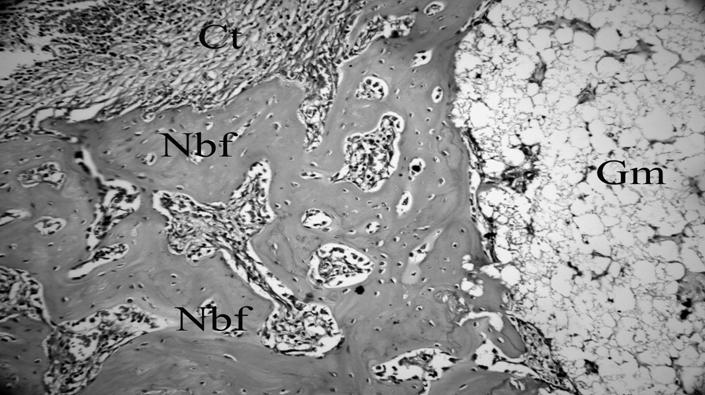
New bone formation and residual graft particles were observed in the histological section taken from the β-TCP group with adjunctive HBOT at four week time point (H&E×200) (Nbf; New bone formation, Gm; Graft material, Ct; Connective tissue).
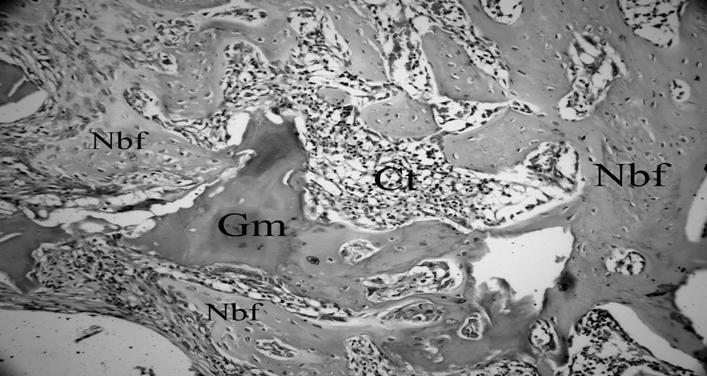
CPCBB graft material which is gradually resorbing and resembles the necrotic bone can be seen in the middle of this slide. This section has been taken from the CPCBB + HBOT group which was sacrified at four week time point (H&E×200) (Nbf; New bone formation, Gm; Graft material, Ct; Connective tissue).
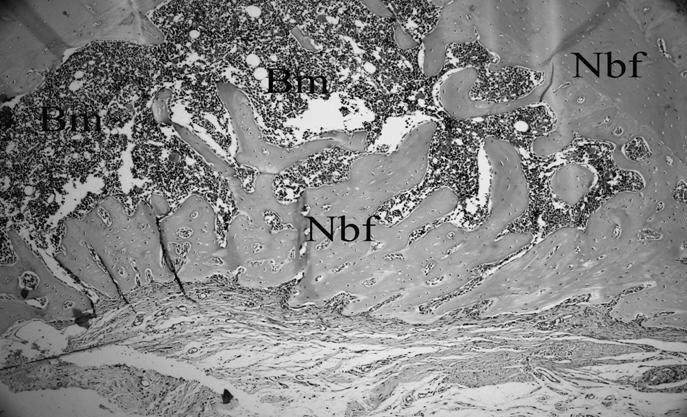
The histological view of the defect which is nearly filled with newly formed bone in the control groups which had received four week of HBOT (H&E×200) (Nbf; New bone formation, Bm; Bone marrow).
Overall results of the bone histomorphometry and serum osteocalcin measurements. Data are presented as mean percentage value and standard deviation (FTF; fibrous tissue formation, CMF; cartilage matrix formation, NBF; new bone formation).
| Variables | Control Groups | ß-Tricalcium Phosphate | Calcium Phosphate Coated Bovine Bone | |||||||
|---|---|---|---|---|---|---|---|---|---|---|
| One week | Two week | Four week | One week | Two week | Four week | One week | Two week | Four week | ||
| FTV (mean%±SD% ) | HBO (-) | 41,4±14,2 | 29,1±9,2 | 14,8±5,2 | 45,2±8,8 | 29,7±13,2 | 30,7±7,4 | 37,7±10,2 | 38,4±11, | 22,5±9,0 |
| HBO (+) | 25±12,1 | 14,5±4,1 | 13,2±10,5 | 35,5±13,4 | 32±6,0 | 26,8±10,1 | 28,7±10,8 | 23,2±10,4 | 17,2±6,9 | |
| CMF (mean%±SD% ) | HBO (-) | 48,1±3,5 | 30,1±18,6 | 19,8±14,4 | 27±15,3 | 33±15,4 | 29,7±13,2 | 16,7±11,1 | 26,4±10,6 | 15,4±7,6 |
| HBO (+) | 13±11,6 | 14,7±9,5 | 8,8±5,4 | 23±11,9 | 17,1±7,8 | 20±8,2 | 9,4±8,3 | 9,8±4,8 | 3,4±1,9 | |
| NBF (mean%±SD% ) | HBO (-) | 16,2±9,9 | 40,2±7,6 | 68,1±10,1 | 9,29±7,7 | 20,7±7,4 | 35,4±10,5 | 21,2±11,0 | 41,8±9,7 | 66,8±9,8 |
| HBO (+) | 19,2±7 | 58,5±12,1 | 71,2±9,4 | 18,7±4,7 | 45,7±11 | 51,8±13,3 | 25,8±10,9 | 53±13,3 | 68,1±6,9 | |
| Osteocalcin ( mean±SD ng/ml) | HBO (-) | 55,1±11 | 37,5±4,7 | 42,1±7,0 | 39,5±6,6 | 38,4±4,2 | 35,1±4,5 | 38,0±5,0 | 38,6±6,4 | 39,1±9,3 |
| HBO (+) | 44,7±5,7 | 49,5±6,5 | 41,3±5,4 | 40,3±6,8 | 45,2±7,9 | 40,8±6,3 | 39,0±6,3 | 40,2±8,1 | 39,4±5,2 | |
Electron microscopy observations
In the ultrastructural evaluation of the periosteum in one and two week specimens in the control groups without HBOT, there were numerous chondroblasts and rarely osteoblasts that contain well-developed intra-cytoplasmic organelles (Figure 5). Among these, the granular endoplasmic reticulum was prominent and golgi apparatus were clearly visible. The chondroblasts were positioned closely, leaving limited intercellular space which also contains dispersed collagen fibrils. In four weeks, osteoblasts with reactive appearance were abundant and the collagen fibrils had became more organized. In B-TCP groups, the general ultrastructural appearance resembles to that of the controls. In addition, it was noted that in some areas the residual graft material had came in contact with the periosteum and the periosteal cells had cytoplasmic process protruded through the bone graft. On the contrary, the ultrastructural investigation of CPCBB groups revealed evidences of severe degeneration both in the intra and extra cellular regions. At one week, normal appearances of the chondroblasts were observed to be altered and these cells also contained degenerated intracellular components. In two and four week specimens, the osteoblast mitochondrion had also lost their usual shape and there were empty intracellular spaces that contain no visible organelles, indicating a vacuolar degeneration process. Moreover, the endoplasmic reticulum membranes were swollen and the nuclei were pyknotic. The collagen fibrils were scarce and they presented a dispersed and disorganized structure.
The ultrastructural findings in the Control + HBOT and B-TCP + HBOT (Figure 6) groups were similar to their non-HBO counterparts with the exceptions of dominant cell types and collagen structure at the early stages of healing. Our observations at one week specimens revealed that the chondroblasts had become scarce and they were mainly replaced by highly active osteoblasts that contain well-developed intracytoplasmic organelles. Additionally, the collagen fibrils appeared to be more organized in bundles. On the other hand, HBOT did not seem to have an effect over the periosteal cell structure of the CPCBB group (Figure 7 a and b) as the cellular degeneration findings were still clearly visible at all time points (Figure 8).
The ultrastructural appearance of two periosteal osteoblast cells with well developed intracytoplasmic organelles in the control group without HBOT at one week time point ( TEM ×6000) (N; Nucleus, Ger; Granular endoplasmic reticulum, Mi; Mitochondrion; Cf; Collagen Fibrils).
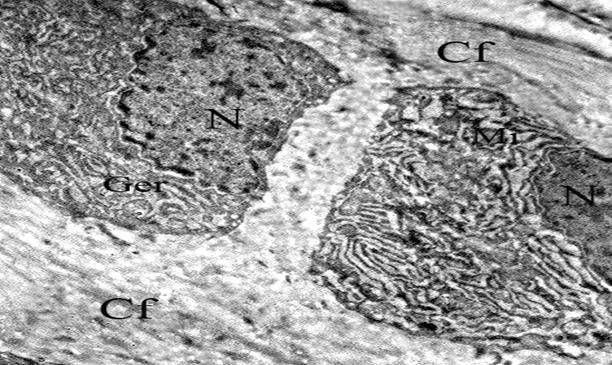
Residual β-TCP bone graft material is seen between two osteoblast cells of the periosteum, note the cytoplasmic processes (arrows) extending from the cell membrane to the bone graft substitute. This electron micrograph was taken from the β-TCP + HBOT group which were sacrificed at one week time point (TEM×7500) (N; Nucleus, R; Ribosome, Ger; Granular Endoplasmic Reticulum).
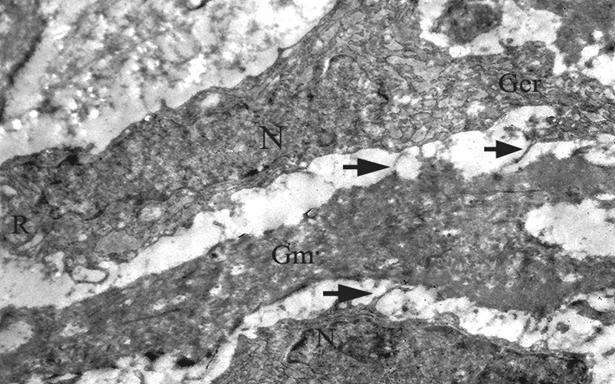
(a) The ultrastructural view of the periosteum in β-TCP group following four week of HBOT. Note well developed membranes of the highly active intracytoplasmic organelles (TEM×6000) (N;Nucleus, Mi; Mitochondrion, Li; Lisosome, Ger; Granular endoplasmic reticulum, Cf; Collagen fibrils) (b) Four week of HBOT could not prevent the damages in the periosteum of the CPCBB group. This electron micrograph shows the extent of degeneration in two periosteal cells. The swollen membranes, the pyknotic nuclei and the dispersed collagen fibrils can be seen as the evidences of deterioration in the cellular structure of this group (TEM×7500) (N; Nucleus, Mi; Mitochondrion, Ger; Granular endoplasmic reticulum, Pli; Phagocytic lisosome, Cf; Collagen Fibrils).
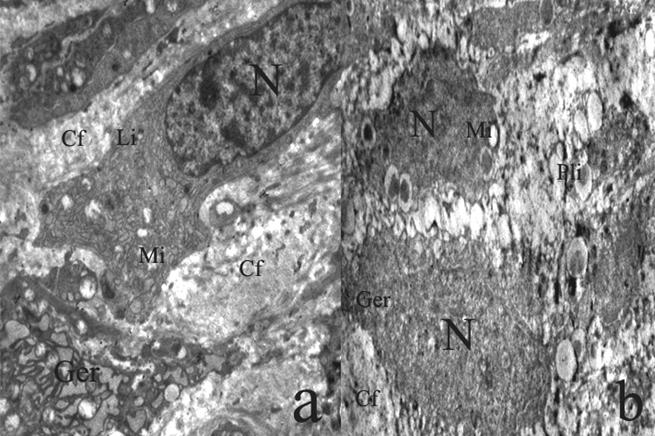
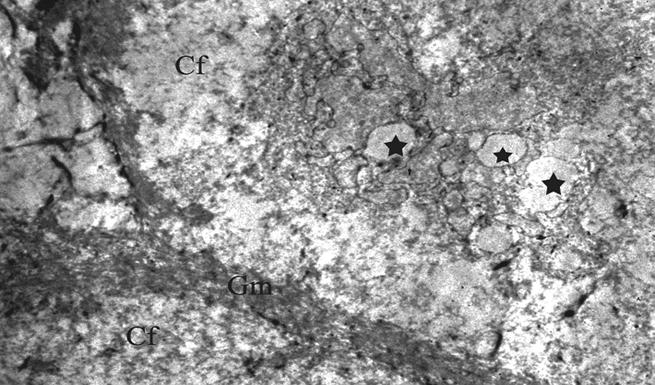
Ultrastructural findings of extensive degeneration in the periosteum of CPCBB + HBOT group at one week time point. It is clear that the the integrity of the cell membrane could not be maintained and there was also evidence of vacuolar degeneration (stars) in the intracytoplasmic compartment (TEM×7500) (Gm; graft material, Cf; Collagen fibrils).
Serum osteocalcin levels
The serum osteocalcin levels were significantly higher in the Control + HBO group (49,5±6,5 ng/ml) when compared to the control animals which did not receive HBOT (37,5±4,7 ng/ml) (p<0.05) at two weeks samples. No significant differences indicating a biochemical effect of HBOT could be found among other groups with respect to the serum osteocalcin levels.
Discussion
Bone tissue is a highly evolved and complex structure which has the ability to heal itself effectively. Therefore, an artificially produced bone substitute should at least present some of its biological properties (20). Characteristics of cell migration, angiogenesis (21) and particle size (22) are among the crucial factors that determine the interaction of the bone grafts with the recipient tissue. During the healing process, precursor cells and different signaling molecules mainly originate from the bone marrow, periosteum and the defect margins (23). New bone formation and angiogenesis are closely related to the extent of tissue oxygenation (24). HBOT has been shown to improve the healing of hard and soft tissue wounds under hypoxic and normal conditions by stimulating angiogenesis and oxygenation (25). Based on this knowledge, our experiments were carried out on a previously studied animal model (26) to which we applied commercially available bone graft materials of similar particle size. Due to the complexity of the bone healing process, we included light microscopic, ultrastuctural and biochemical analysis in our study. To easily detect possible histological and biochemical changes, we selected our harvest time points according to previous reports indicating higher cellular activity at these days (27). Similarly, our HBOT protocol was derived from clinical studies in which this procedure had been reported to demonstrate high therapeutic efficiency without any side effects (28).
The effects of various HBOT protocols on the healing of normally perfused bone injuries have been extensively investigated using different experimental settings. In the earlier studies, the adjunctive HBOT was found to improve the calcium binding and resistance of femur fractures (29) and also the torsional strength of distracted rabbit tibiae(30)Nilsson et al. (31) compared the influences of heparin, dextrane and HBOT in preventing soft and hard tissue damages in experimentally created vertical ramus osteotomies. They reported that the ten days 2,8 ATA once daily 80 minutes of HBOT, had suppressed the inflammation and also increased the fusion rate of fractures when compared to the groups without HBOT. Same authors (32) also evaluated the hard tissue deposition around an implanted bone harvest chamber and they observed a significant increase in the new bone formation following three weeks 2,8 ATA once daily 120 minutes of HBOT. Penttinen et al.(33)investigated the effects of 2,5 ATA twice daily 120 minutes of HBOT on experimentally created rat femur fractures. They reported that the fracture mineralization was higher in HBOT given rats at two weeks, when compared to the non-HBOT animals. Histopathologically, they observed hypertrophic chondrocytes and significant new bone formation in HBOT groups at the same time point. More recently, Jan et al.(34)investigated the effects of 2,4 ATA once daily 90 minutes of HBOT for 20 days on the healing of rabbit critical size calvarial defect model in which the animals were sacrificed at six and 12 weeks time points. They observed that the HBOT group produced a tissue regenerate with many blood vessels and cellular marrow spaces. Also, their histomorphometric analysis demonstrated more bone formation in the HBOT group when compared to the non-HBOT animals. Although these previous reports were not directly comparable with our results due to the inconsistency of animal models and HBOT procedures, our findings showed a similar pattern in the healing of control defects in rats given HBOT. In light microscopy, we observed an increase in the new bone formation as well as less fibrous tissue and cartilage matrix in HBOT given control animals at one and two weeks specimens. These subjective findings were also confirmed to some extent with bone histomorphometry. In the ultrastructural analysis, the periosteum of HBOT groups was observed to contain active osteoblasts and well-organized collagen fibrils when compared to the chondroblast dominated and dispersed collagenous structure in the non-HBOT groups. Furthermore, new bone formation had become detectable biochemically in the HBOT given rats, as the serum osteocalcin levels were significantly higher than the non-HBOT group at two weeks serum samples. Therefore, we think that the HBOT contributed positively to the healing process of empty defects in rat tibiae.
Tricalcium phosphate based bone substitutes and particulated bovine bone grafts were histologically compared in a number of experimental studies which produced conflicting results (35,36). In our study, we observed that the defects filled with CPCBB showed a more regular new bone apposition-material resorption pattern when compared to the β-TCP. Also, at four weeks, the healing of these defects was similar to that of the control group. On the other hand, our ultrastructural investigation revealed that the CPCBB caused severe degeneration in both extra and intracellular components of the periosteum with no apparent clinical signs of inflammation or infection. In contrast, the β-TCP particles had acceptable integration with periosteal cells. These interesting and previously unreported findings suggest the necessity of multidisciplinary study designs which take into account different characteristics of the tissues involved in host tissue - bone graft interactions.
The use of adjunctive HBOT to improve bone healing in autogenous bone transplants has been investigated in the histologic observation of the iliac grafts placed in mandibular defects of animals revealed that 2,4 ATA 60 minutes twice daily (20 sessions before 10 sessions after the surgery) HBOT encouraged new vessel formation at one week and new bone deposition at two week time points (37) Additionally, the spinal fusion rate and torsional strength have been found to be higher in a rabbit postero-lateral intertranverse fusion model with adjunctive HBOT(38). This treatment modality has also been shown to increase bone formation, serum alkaline phosphatase activity and calcium levels when bone morphogenetic proteins were implanted to normally perfused (39) or ischemic regions (40) in a rat model. Jan et al.(41) reported that the unfilled critical-size calvarial defects in animals exposed to HBOT had less fibrous tissue, more new bone and marrow formations than unfilled non-HBOT defects. However, they did not find any statistical difference in bone formation parameters between defects grafted with autogenous bone in non-HBOT and HBOT groups. When similar defects were filled with demineralized bone matrix (DBM) or biphasic calcium phosphate (BCP) bone substitutes and exposed to 20 sessions 2,4 ATA once daily 90 minutes of HBOT (42), a significant increase in the new bone formation in DBM-grafted sites and less fibrous tissue in BCP implanted defects were observed. Our histomorphometric findings also revealed less fibrous tissue in CPCBB + HBOT groups. In addition, we found that the cartilaginous matrix formation significantly decreased in all groups. Between two grafting materials, the HBOT promoted new bone formation only in β-TCP filled defects at one and two week time points. However, the overall healing in these defects was still inferior to controls and CPCBB groups with or without HBOT.
Different healing patterns observed with two bone substitutes in response to the same HBOT procedure could be partially explained by the basic tissue effects of HBOT and local characteristics of the bone grafts. Collagen synthesis from fibroblasts and the formation of osteoid substance by osteoblasts are both oxygen-dependent processes (43). Vascular disruption and hypoxia are natural consequences of the bone defects which, if extended, could change the overall healing pattern (44). Hypoxia promotes chondrocytic differentiation and cartilage matrix synthesis (45). Therefore, the collagen tissue organization and early osteoblast detection in periosteum as well as new bone, less fibrous and less cartilage tissue formations in the defects of animals exposed to HBOT may be related to the increased partial pressure and transportation of oxygen in HBOT groups. On the other hand, larger gaps between the β-TCP particles which were observed to be filled with connective tissue could have provided more space for the new bone in growth related to HBOT, whereas the intact but steadily resorptive structure and/or the degeneration in periosteum of CPCBB specimens could have limited the effects of HBOT on these groups. From this point of view, these findings could also suggest that the successful interaction of a bone graft substitute with the host tissue under normobaric conditions may not be indicative of the similar process under hyperbaric environment.
Conclusion
HBOT has led to an increase in new bone formation and improved the cellular structure as well as the collagen fibril organization in the periosteum of the unfilled and β-TCP filled defects. This process was also biochemically detectable in the control group. Generally, HBOT resulted in a reduction in fibrous tissue and cartilage matrix formation but it was not prominently effective in the healing of CPCBB filled defects.
Acknowledgements
This study has been supported by a research fund of Istanbul University. Project number is T - 274 / 18062003.
Conflict of Interest
The authors have declared that no conflict of interest exists.
References
1. Gupta MC, Maitra S. Bone grafts and bone morphogenetic proteins in spine fusion. Cell Tissue Bank. 2002;3:255-267
2. Nasr HF, Aichelmann-Reidy ME, Yukna RA. Bone and bone substitutes. Periodontol 2000. 1999;19:74-86
3. Nassr A, Khan MH, Ali MH, Espiritu MT, Hanks SE, Lee JY. et al. Donor-site complications of autogenous nonvascularized fibula strut graft harvest for anterior cervical corpectomy and fusion surgery: experience with 163 consecutive cases. Spine J. 2009;9:893-898
4. Khan Y, Yaszemski MJ, Mikos AG, Laurencin CT. Tissue engineering of bone: material and matrix considerations. J Bone Joint Surg Am. 2008;90(Suppl 1):36-42
5. Kamitakahara M, Ohtsuki C, Miyazaki T. Review paper: behavior of ceramic biomaterials derived from tricalcium phosphate in physiological condition. J Biomater Appl. 2008;23:197-212
6. De CP, Browaeys H, De BH. Healing of Extraction Sockets Filled with BoneCeramic(R) Prior to Implant Placement: Preliminary Histological Findings. Clin Implant Dent Relat Res. 2011;13:34-45
7. Dori F, Huszar T, Nikolidakis D, Tihanyi D, Horvath A, Arweiler NB. et al. Effect of platelet-rich plasma on the healing of intrabony defects treated with Beta tricalcium phosphate and expanded polytetrafluoroethylene membranes. J Periodontol. 2008;79:660-669
8. Uckan S, Deniz K, Dayangac E, Araz K, Ozdemir BH. Early Implant Survival in Posterior Maxilla With or Without beta-Tricalcium Phosphate Sinus Floor Graft. J Oral Maxillofac Surg. 2010Jul;68(7):1642-5
9. Hislop WS, Finlay PM, Moos KF. A preliminary study into the uses of anorganic bone in oral and maxillofacial surgery. Br J Oral Maxillofac Surg. 1993;31:149-153
10. Precheur HV. Bone graft materials. Dent Clin North Am. 2007;51:729-46
11. Hallman M, Lundgren S, Sennerby L. Histologic analysis of clinical biopsies taken 6 months and 3 years after maxillary sinus floor augmentation with 80% bovine hydroxyapatite and 20% autogenous bone mixed with fibrin glue. Clin Implant Dent Relat Res. 2001;3:87-96
12. Artzi Z, Nemcovsky CE, Tal H. Efficacy of porous bovine bone mineral in various types of osseous deficiencies: clinical observations and literature review. Int J Periodontics Restorative Dent. 2001;21:395-405
13. Carmagnola D, Berglundh T, Araujo M, Albrektsson T, Lindhe J. Bone healing around implants placed in a jaw defect augmented with Bio-Oss. An experimental study in dogs. J Clin Periodontol. 2000;27:799-805
14. Jain KK. Physical, physiological and biochemical aspects of hyperbaric oxygenation. In: (ed.) Jain KK, Neubauer R, Correa JG. The Textbook of Hyperbaric Medicine. Toronto: Hogrefe and Huber Publishers. 1990:335-365
15. David JC. et al. Hyperbaric medicine: Patient selection, treatment procedures and side effects. In: (ed.) Davis JC, Hunt TK. Problemwounds The role of oxygen. New York: Elsevier. 1988:225-235
16. Vudiniabola S, Pirone C, Williamson J, Goss AN. Hyperbaric oxygen in the prevention of osteoradionecrosis of the jaws. Aust Dent J. 1999;44:243-247
17. van SD, Naert I, Bossuyt M, De MG, Calberson L, Ghyselen J. et al. The rehabilitation of the severely resorbed maxilla by simultaneous placement of autogenous bone grafts and implants: a 10-year evaluation. Clin Oral Investig. 1997;1:102-108
18. Sclaroff A, Haughey B, Gay WD, Paniello R. Immediate mandibular reconstruction and placement of dental implants. At the time of ablative surgery. Oral Surg Oral Med Oral Pathol. 1994;78:711-717
19. Goiato MC, Santos DM, Danelon M, Pesqueira AA, de Carvalho Dekon SF, Fajardo RS. Hyperbaric oxygen: therapy for patients with maxillofacial implants? J Craniofac Surg. 2009;20:1519-1522
20. Burg KJ, Porter S, Kellam JF. Biomaterial developments for bone tissue engineering. Biomaterials. 2000;21:2347-2359
21. Henno S, Lambotte JC, Glez D, Guigand M, Lancien G, Cathelineau G. Characterisation and quantification of angiogenesis in beta-tricalcium phosphate implants by immunohistochemistry and transmission electron microscopy. Biomaterials. 2003;24:3173-3181
22. Zhou X, Zhang Z, Li S, Bai Y, Xu H. Osteoconduction of different sizes of anorganic bone particles in a model of guided bone regeneration. Br J Oral Maxillofac Surg. 2011Jan;49(1):37-41
23. Bush D, England B, Tucci M, Cason Z, Lemos L, Benghuzzi H. The effect of TCPL devices on tissue-implant interface analysis using adult sheep as a model. Biomed Sci Instrum. 1995;31:147-152
24. Carano RA, Filvaroff EH. Angiogenesis and bone repair. Drug Discov Today. 2003;8:980-989
25. Fulton JEJr. The use of hyperbaric oxygen (HBO) to accelerate wound healing. Dermatol Surg. 2000;26:1170-1172
26. Stevenson S, Emery SE, Goldberg VM. Factors affecting bone graft incorporation. Clin Orthop Relat Res. 1996:66-74
27. Landry PS, Marino AA, Sadasivan KK, Albright JA. Bone injury response. An animal model for testing theories of regulation. Clin Orthop Relat Res. 1996:260-273
28. Barth E, Sullivan T, Berg E. Animal model for evaluating bone repair with and without adjunctive hyperbaric oxygen therapy (HBO): comparing dose schedules. J Invest Surg. 1990;3:387-392
29. Coulson DB, Ferguson ABJr, Diehl RCJr. Effect of hyperbaric oxygen on the healing femur of the rat. Surg Forum. 1966;17:449-450
30. Ueng SW, Lee SS, Lin SS, Wang CR, Liu SJ, Yang HF. et al. Bone healing of tibial lengthening is enhanced by hyperbaric oxygen therapy: a study of bone mineral density and torsional strength on rabbits. J Trauma. 1998;44:676-681
31. Nilsson LP, Granstrom G, Rockert HO. Effects of dextrans, heparin and hyperbaric oxygen on mandibular tissue damage after osteotomy in an experimental system. Int J Oral Maxillofac Surg. 1987;16:77-89
32. Nilsson P, Albrektsson T, Granstrom G, Rockert HO. The effect of hyperbaric oxygen treatment on bone regeneration: an experimental study using the bone harvest chamber in the rabbit. Int J Oral Maxillofac Implants. 1988;3:43-48
33. Penttinen R, Niinikoski J, Kulonen E. Hyperbaric oxygenation and fracture healing. A biochemical study with rats. Acta Chir Scand. 1972;138:39-44
34. Jan AM, Sandor GK, Iera D, Mhawi A, Peel S, Evans AW. et al. Hyperbaric oxygen results in an increase in rabbit calvarial critical sized defects. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;101:144-149
35. Jensen SS, Broggini N, Hjorting-Hansen E, Schenk R, Buser D. Bone healing and graft resorption of autograft, anorganic bovine bone and beta-tricalcium phosphate. A histologic and histomorphometric study in the mandibles of minipigs. Clin Oral Implants Res. 2006;17:237-243
36. Schwartz Z, Doukarsky-Marx T, Nasatzky E, Goultschin J, Ranly DM, Greenspan DC. et al. Differential effects of bone graft substitutes on regeneration of bone marrow. Clin Oral Implants Res. 2008;19:1233-1245
37. Sawai T, Niimi A, Takahashi H, Ueda M. Histologic study of the effect of hyperbaric oxygen therapy on autogenous free bone grafts. J Oral Maxillofac Surg. 1996;54:975-981
38. Chen WJ, Lai PL, Chang CH, Lee MS, Chen CH, Tai CL. The effect of hyperbaric oxygen therapy on spinal fusion: using the model of posterolateral intertransverse fusion in rabbits. J Trauma. 2002;52:333-338
39. Okubo Y, Bessho K, Fujimura K, Kusumoto K, Ogawa Y, Iizuka T. Effect of hyperbaric oxygenation on bone induced by recombinant human bone morphogenetic protein-2. Br J Oral Maxillofac Surg. 2001;39:91-95
40. Okubo Y, Bessho K, Fujimura K, Kusumoto K, Suzuki T, Segami N. et al. Preclinical study of recombinant human bone morphogenetic protein-2: application of hyperbaric oxygenation during bone formation under unfavourable condition. Int J Oral Maxillofac Surg. 2003;32:313-317
41. Jan A, Sandor GK, Brkovic BB, Peel S, Evans AW, Clokie CM. Effect of hyperbaric oxygen on grafted and nongrafted calvarial critical-sized defects. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009;107:157-163
42. Jan A, Sandor GK, Brkovic BB, Peel S, Kim YD, Xiao WZ. et al. Effect of hyperbaric oxygen on demineralized bone matrix and biphasic calcium phosphate bone substitutes. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2010;109:59-66
43. Hunt TK. The physiology of wound healing. Ann Emerg Med. 1988;17:1265-1273
44. Gottrup F. Oxygen in wound healing and infection. World J Surg. 2004;28:312-315
45. Hirao M, Tamai N, Tsumaki N, Yoshikawa H, Myoui A. Oxygen tension regulates chondrocyte differentiation and function during endochondral ossification. J Biol Chem. 2006;281:31079-31092
Author contact
![]() Corresponding author: Dr. Yigit Sirin, Istanbul Universitesi, Dishekimligi Fakultesi, Agiz-Dis Cene Hast. Ve Cerr.Anabilim Dali 34390, Capa/Fatih/Istanbul. +902124142020/30289; ysirinedu.tr
Corresponding author: Dr. Yigit Sirin, Istanbul Universitesi, Dishekimligi Fakultesi, Agiz-Dis Cene Hast. Ve Cerr.Anabilim Dali 34390, Capa/Fatih/Istanbul. +902124142020/30289; ysirinedu.tr

 Global reach, higher impact
Global reach, higher impact