Impact Factor ISSN: 1449-1907
Int J Med Sci 2023; 20(6):781-796. doi:10.7150/ijms.75315 This issue Cite
Research Paper
SOX2 Promotes Radioresistance in Non-small Cell Lung Cancer by Regulating Tumor Cells Dedifferentiation
1. Department of Oncology, Tongji Hospital, Tongji Medical College of Huazhong University of Science and Technology, Wuhan, China
2. Xiangyang Central Hospital, Xiangyang, China
#These authors contributed equally to this work.
Abstract
Background: Radiation therapy plays an important role in the treatment of patients with non-small cell lung cancer (NSCLC). However, the radiocurability is greatly limited because of radioresistance which leads to treatment failure, tumor recurrence, and metastasis. Cancer stem cell (CSC) has been identified as the main factor that contributes to radiation resistance. SOX2, one of the transcription factors specifically expressed in CSC, is involved in tumorigenesis, progression, and maintenance of cell stemness. But the association between SOX2 and NSCLC radioresistance is not clear now.
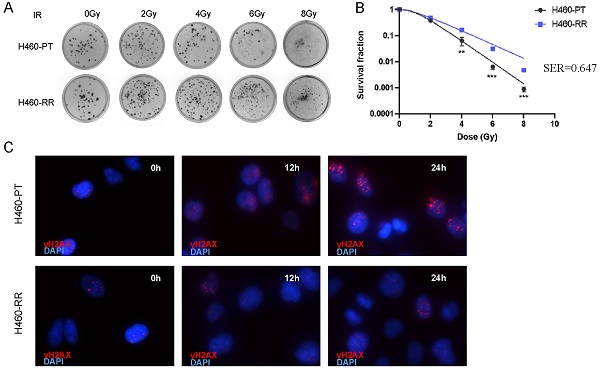
Methods: We constructed the radiotherapy-resistant cell line of NSCLC by multiple radiotherapy treatments. Colony formation assay, western blot, and immunofluorescence were performed to detect the radiosensitivity of cells. Western blot, qRT-PCR, and sphere formation assay were used to detect CSC characteristics of cells. Wound healing assay and Transwell assay were used to determine cell migration motility. The SOX2-upregulated model and SOX2-downregulated model was constructed by lentivirus transduction. Finally, the expression and clinical relevance of SOX2 in NSCLC were investigated by bioinformatics analysis based on TCGA and GEO datasets.
Results: The expression of SOX2 was increased in radioresistant cells and a trend of dedifferentiation were observed. The results of wound healing assay and Transwell assay showed that SOX2 overexpression significantly promote the migration and invasion of NSCLC cells. Mechanistically, overexpression of SOX2 enhanced radioresistance and DNA damage repair capability of parental cells, while down-regulation of SOX2 led to decreased radioresistance and DNA repair ability in radioresistant cells, all of which were related to cells dedifferentiation regulated by SOX2. In addition, bioinformatics analysis show that high expression of SOX2 was strongly associated with the progression and poor prognosis of patients with NSCLC.
Conclusions: Our study revealed that SOX2 regulates radiotherapy resistance in NSCLC via promoting cell dedifferentiation. Therefore, SOX2 may be a promising therapeutic target for overcoming radioresistance in NSCLC, providing a new perspective to improve the curative effect.
Keywords: Non-small cell lung cancer, radioresistance, cancer stem cell, SOX2

 Global reach, higher impact
Global reach, higher impact