Impact Factor
ISSN: 1449-1907
Int J Med Sci 2022; 19(10):1519-1524. doi:10.7150/ijms.67083 This issue Cite
Research Paper
The length of stay and inpatient burden in inpatients with different psoriasis subtypes
1. Department of Dermatology, Xiangya Hospital, Central South University, Changsha, China 410008.
2. National Clinical Research Center for Geriatric Disorders (Xiangya Hospital), Changsha, China 410008.
3. Hunan Engineering Research Center of Skin Health and Disease; Hunan Key Laboratory of Skin Cancer and Psoriasis (Xiangya Hospital), Changsha, China 410008.
4. Hospital for Skin Diseases, Institute of Dermatology, Chinese Academy of Medical Sciences & Peking Union Medical College, Nanjing, China 210042.
5. Department of Information, Xiangya Hospital, Central South University, Changsha, China 410008.
Abstract
Background: Heavy disease burden of psoriasis has been indicated by previous studies. However, the cost of care and length of stay (LOS) in inpatients with different psoriasis subtypes were rarely addressed. This study aimed to investigate the cost of care and LOS in Chinese patients with different psoriasis types and to clarify the independent factors affecting LOS.
Methods: We conducted a cross-sectional study by enrolling patients with psoriasis who were hospitalized between 13 Feb 2017 and 29 Mar 2021. Demographic and clinical characteristics of the patients were collected by reviewing their Electronic Medical Records. Multivariate linear regression was used to estimate the associations with adjustments.
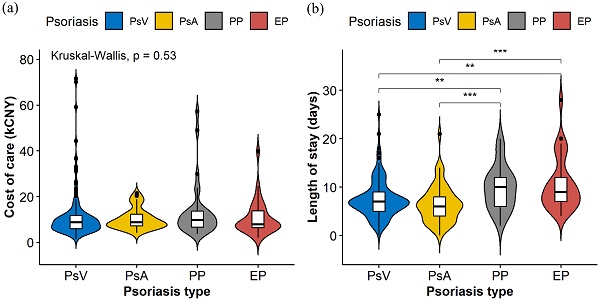
Results: A total of 310 adult patients with psoriasis were included (mean cost of care: 13.0±22.3 kCNY; mean LOS: 7.9±4.3 days). Statistically significant differences were found among patients with different psoriasis subtypes in LOS (P<0.001) but not in the cost of care (P=0.530). Relative to psoriasis vulgaris, pustular psoriasis (Adjusted coefficient: 2.37, 95% confidence interval (CI): 0.87-3.87) and erythrodermic psoriasis (Adjusted coefficient: 2.92, 95%CI: 1.38-4.47) were significantly associated with an increased LOS. Meanwhile, respiratory tract infections (Adjusted coefficient: 1.60, 95%CI: 0.11-3.10) also significantly increased the LOS. On the contrary, a decreased LOS was found in psoriatic arthritis patients treated with TNF-alpha inhibitors (Adjusted coefficient: -2.21, 95%CI: -4.37 to -0.05).
Conclusions: LOS differed significantly among different psoriasis subtypes while the inpatient burden for a single hospitalization was alike. Infection is an important factor associated with a longer LOS. TNF-alpha inhibitors evidently reduced the total hospital stay period for patients with psoriatic arthritis.
Keywords: inpatient, length of stay, burden, cost of care, psoriasis, psoriatic arthritis

 Global reach, higher impact
Global reach, higher impact