Impact Factor ISSN: 1449-1907
Int J Med Sci 2021; 18(12):2599-2606. doi:10.7150/ijms.59698 This issue Cite
Research Paper
Urate-lowering Therapy and Chronic Kidney Disease Development in Patients with Gout
1. Dr. Yen's Clinic, Taoyuan City, Taiwan.
2. Institute of Medicine, Chung Shan Medical University, Taichung, Taiwan.
3. Department of Medicine, Chung Shan Medical University Hospital, Taichung, Taiwan.
4. Graduate Institute of Integrated Medicine, China Medical University, Taichung, Taiwan.
5. Management Office for Health Data, China Medical University Hospital, Taichung City, Taiwan.
6. Graduate Institute of Clinical Medical Science, College of Medicine, China Medical University, Taichung City, Taiwan.
7. Institute of Environmental & Occupational Health Sciences, School of Medicine, National Yang-Ming University, Taipei, Taiwan.
8. Institute of Public Health, School of Medicine, National Yang-Ming University, Taipei, Taiwan.
9. Division of Clinical Toxicology & Occupational Medicine, Department of Medicine, Taipei Veterans General Hospital, Taipei, Taiwan.
10. Institute of Population Health Sciences, National Health Research Institutes, Zhunan, Miaoli, Taiwan.
11. Department of Health Services Administration, China Medical University, Taichung, Taiwan.
12. Department of Family Medicine, Min-Sheng General Hospital, Taoyuan, Taiwan.
13. Faculty of Medicine, National Yang-Ming University School of Medicine, Taipei, Taiwan.
14. Section of Endocrinology and Metabolism, Department of Medicine, Taipei Veterans General Hospital, Taipei, Taiwan.
#These authors contributed equally to this work.
Abstract
Objectives: Chronic kidney disease (CKD) has emerged as a global health concern. Many studies have identified an association between hyperuricemia and CKD, and some studies have revealed that urate-lowering therapy (ULT) can attenuate CKD progression. However, only a few studies have explored the role of ULT in the prevention of new onset CKD.
Methods: To compare the risk of incident CKD between users and nonusers of ULT in patients with gout, we conducted a 13-year population-based retrospective cohort study. Overall incidence of CKD was compared between 7126 ULT users and 7126 matched ULT nonusers.
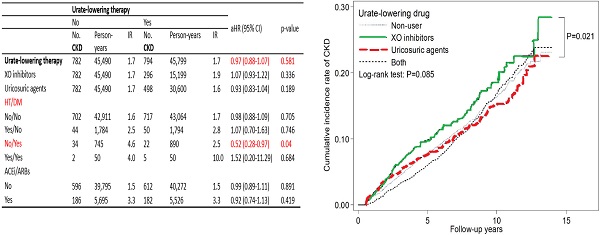
Results: The CKD incidence rate for both the users and nonusers of ULT was 1.7 per 100 person-years, after adjusting for sex, age, region of residence, comorbidities, and medications used. No significant difference in CKD risk (adjusted hazard ratio [aHR]: 0.97; 95% confidence interval [CI]: 0.88-1.07) was noted between the ULT users and nonusers. In the subgroup of patients with diabetes mellitus (DM) and without hypertension (HT), ULT tended to be associated with lower risk of incident CKD (aHR: 0.52; 0.95% CI: 0.28-0.97). Compared with the risk of new onset CKD in patients receiving xanthine oxidase inhibitors, those receiving uricosuric agents seemed to have a lower risk of developing CKD (aHR: 0.81, 95% CI: 0.67-0.99).
Conclusion: This population-based cohort study indicated that ULT is not associated with lower risk of CKD development. However, in the subgroup of patients with DM and without HT, ULT is associated with significantly lower risk of incident CKD.
Keywords: gout, urate-lowering therapy, chronic kidney disease, diabetes mellitus, hypertension

 Global reach, higher impact
Global reach, higher impact