Impact Factor ISSN: 1449-1907
Int J Med Sci 2021; 18(11):2339-2346. doi:10.7150/ijms.57886 This issue Cite
Research Paper
Impact of pentraxin 3 genetic variants on uterine cervical cancer clinicopathologic characteristics
1. Institute of Medicine, Chung Shan Medical University, Taichung, Taiwan.
2. Department of Obstetrics and Gynecology, Chi-Mei Foundation Medical Center, Tainan, Taiwan.
3. Department of Medical Imaging and Radiological Sciences, Chung Shan Medical University, Taichung, Taiwan.
4. Department of Radiation Oncology, Chung Shan Medical University Hospital, Taichung, Taiwan.
5. Department of Medicine, National Taiwan University, Taipei, Taiwan.
6. School of Medicine, Chung Shan Medical University, Taichung, Taiwan.
7. Department of Obstetrics and Gynecology, Changhua Christian Hospital, Changhua, Taiwan.
8. Department of Obstetrics and Gynecology, Chiayi Chang Gung Memorial Hospital Chiayi, Taiwan.
9. Department of Nursing, Chang Gung University of Science and Technology, Chiayi Campus, Chiayi, Taiwan.
10. Department of Medical Research, Chung Shan Medical University Hospital, Taichung, Taiwan.
11. Department of Obstetrics and Gynecology, Chung Shan Medical University Hospital, Taichung, Taiwan.
#Equal contribution as first authors.
Abstract
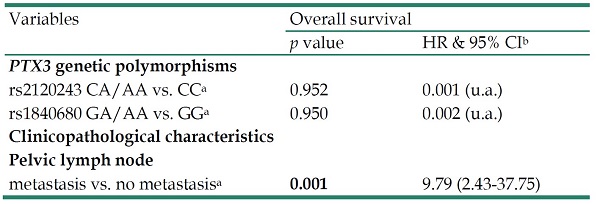
The aims of this study were to investigate the relationships among pentraxin 3 (PTX3) genetic variants and development and clinicopathological characteristics of uterine cervical cancer, and patient survival in Taiwanese women. The study enrolled 125 patients with invasive cancer and 98 patients with precancerous lesions of uterine cervix, and 325 control women. PTX3 genetic variants rs2120243, rs3816527, rs2305619 and rs1840680 were selected and their genotypic distributions were determined by real-time polymerase chain reaction. Our results indicated that patients with genotype CC in PTX3 rs2120243 and genotype GG in rs1840680 had more chance to have adenocarcinoma but not squamous cell carcinoma, as compared to those with CA/AA and those with GA/AA, respectively. No other clinicopatholgical characteristics were associated with PTX3 genetic variants. In addition, PTX3 genetic variants were not associated with 5 years survival of cervical cancer patients. In conclusions, PTX3 genetic variants are not associated with carcinogenesis and clinicopathological variables of uterine cervix and patient survival in Taiwanese women. The only independent predictor for the 5 years survival is pelvic lymph node metastasis.
Keywords: pentraxin 3, genetic variants, uterine cervical cancer, pelvic lymph node metastasis

 Global reach, higher impact
Global reach, higher impact