Impact Factor ISSN: 1449-1907
Int J Med Sci 2010; 7(6):358-365. doi:10.7150/ijms.7.358 This issue Cite
Research Paper
Pravastatin Provides Antioxidant Activity and Protection Of Erythrocytes Loaded Primaquine
1. Kayyali Chair for Pharmaceutical Industry, Department of Pharmaceutics, College of Pharmacy, King Saud University, P.O. Box 2457, Riyadh 11451, Saudi Arabia.
2. Center of Excellence in Biotechnology Research, King Saud University, P.O. Box 2460, Riyadh, 11451, Saudi Arabia.
Received 2010-9-2; Accepted 2010-10-27; Published 2010-10-28
Abstract
Loading erythrocytes with Primaquine (PQ) is advantageous. However, PQ produces damage to erythrocytes through free radicals production. Statins have antioxidant action and are involved in protective effect against situation of oxidative stress. Thus the protective effect of pravastatin (PS) against PQ induced oxidative damage to human erythrocytes was investigated in the current studies upon loading to erythrocytes.
The erythrocytes were classified into; control erythrocytes, erythrocytes incubated with either 2 mM of PS or 2 mM of PQ, and erythrocytes incubated with combination of PS plus PQ. After incubation for 30 min, the effect of the drugs on erythrocytes hemolysis as well as some biomarkers of oxidative stress (none protein thiols, protein carbonyl, thiobarbituric acid reactive substance) were investigated.
Our results revealed that PS maintains these biomarkers at values similar to that of control ones. On the other hand, PQ cause significant increases of protein carbonyl by 115% and thiobarbituric acid reactive substance by 225% while non-protein thiols were significantly decreased by 112 % compared with control erythrocytes. PS pre-incubation before PQ exerts marked reduction of these markers in comparison with PQ alone. Moreover, at NaCl concentrations between 0.4% and 0.8%, PQ causes significant increase of Red Blood Cells (RBCs) hemolysis in comparison with the other groups (P<0. 001). Scanning electron micrograph indicates spherocytes formation by PQ incubation, but in the other groups the discocyte shape of erythrocytes was preserved.
The reduction of protein oxidation and lipids peroxidation by PS is related to antioxidants effect of this statin. Preservation of erythrocytes fragility and morphology by PS are related to its free radicals scavenging effect. It is concluded that pravastatin has protective effect against erythrocytes dysfunction related any situations associated with increased oxidative stress, especially when loaded with PQ.
Keywords: Erythrocytes, Drug delivery, Pravastatin, Primaquine, Oxidative Stress.
Introduction
Erythrocytes as drug delivery systems (DDS's) are exposed to several stress situations. This stress may be either physical, hyperosmotic, as well as oxidative stress [1]. The erythrocytes membrane is protected from oxidative damages by antioxidant enzymes system such as superoxide dismutase, catalase, and glutathione peroxidase in addition to non enzymatic systems such as glutathione, vitamins A, C and E [2]. The alteration of these protective mechanisms may result in increase of free radicals production that alters the cellular functions [3].
RBCs are frequently exposed to oxygen when loaded with drugs as DDS's, thus are more susceptible to oxidative damage. Moreover, the hemoglobin in RBCs is a strong catalyst that may initiate oxidative damage [4]. Oxidation of erythrocytes leads to significant alterations in their structural lipids as well as deformations of the cytoskeletal proteins [5]. In addition to lipid peroxidation, sulfhydryl groups of proteins may be targeted for oxidative stress [4]. Furthermore, the decrease of glutathione can enhance the tendency of sulfhydryl groups to oxidation [5]. Oxidation of proteins increases the formation of disulfide as well as carbonyl groups [6].
Toxic manifestations induced by several drugs are shown to be mediated by oxidative stress mechanisms. Involvement of reactive oxygen species (ROS) has been demonstrated in the toxicity of many drugs to erythrocytes [7]. PQ is used for treatment of malarial infections and its loading to erythrocytes is useful. The therapeutic use of this drug is restricted due to its toxic side effects. PQ causes hemolytic anemia especially in glucose-6-phosphate dehydrogenase deficient patients [8]. The interaction between PQ with reduced nicotinamide dinucleotide phosphate (NADPH) underlies many aspects of PQ toxicity. Also, the autooxidation of PQ result in formation of ROS which leading to oxidative alterations in erythrocytes [9]. These species not only overwhelm cellular antioxidant defenses but also attack cellular structural molecules, leading to oxidative modification of erythrocytes [10].
Antioxidants can help in preservation of an adequate antioxidant status; therefore, they preserve the normal physiological function of living cells by protection against reactive oxygen species [11]. Statins are the group of drugs that lower the blood cholesterol level, besides their therapeutic uses of hyperlipidemia, inflammation, immunomodulation in addition to antioxidant effects [12, 13]. Pravastatin (PS) is one of the statins group effective in the treatment of hypercholesterolemia. Moreover, it has other beneficial effects on several cardiovascular alterations [14]. Previously the study demonstrated that treatment with PS has protective effect against oxidative stress [15].
The present study was designed to demonstrate the protective effect of PS against PQ induced lipids peroxidation, proteins oxidation as well as hemolysis of human erythrocytes upon loading. The erythrocytes are incubated with PQ for 30 min and its effect on erythrocytes thiobarbituric acid reactive substance (TBARS), protein carbonyl (PCO) as well as non-protein thiols (NPSH) is determined in presence and absence of PS.
Materials and methods
Materials
Pravastatin sodium was gifted by Saudi Pharmaceutical Industries & Medical Appliances Corporation (SPIMACO, Al-Qassim, Saudi Arabia). Primaquine diphosphate, Ellman's reagent and thiobarbituric acid, tetraethoxypropane were provided by Sigma Chemical Co., St. Louis, MO, USA. Acetonitrile, methanol, isopropanol, trichloroacetic acid and sodium hydroxide were supplied by Merck Germany. 2,4-Dinitrophenylhydrazine and, Guanidine hydrochloride were obtained from (BDH Chemical Ltd Poole UK, and Winlab, UK respectively. All of the remaining chemicals used in the studies are commercially available as analytical grade.
Instrumentation
Spectro UV-Vis Split Beam PC (Model UVS-2800, Labomed, Inc.); Shaking Water Bath (Julabo SW22); Centrifuge CT5 were used for the investigation of the present studies and COULTER® LH 780 is used as Hematology Analyzer.
Specimen collection and erythrocytes isolation
Blood samples were collected in heparinized tubes from adult men (ages between 35-40 years) not suffered from chronic or acute illness. Informed consent was obtained from all donors. The blood was centrifuged for 5 min at 1500 rpm. The plasma and buffy coat were removed by aspiration to eliminate leucocytes and platelets; erythrocytes were washed three times in cold phosphate buffer saline pH 7.4 with centrifugation for 5 min at 1500 rpm [16]. This study was approved by the research center ethics committee of College of Pharmacy, King Saud University, Riyadh, Saudi Arabia.
Experimental design
Erythrocytes suspension with hematocrite adjusted at 45% were classified into 4 groups where each group contains 6 samples: in group one the erythrocytes exposed neither pravastatin nor primaquine (control group). In the second group, the erythrocytes were incubated with 2mM of pravastatin. The erythrocytes were treated with 2mM of primaquine in the third group. And in the fourth group the erythrocytes were exposed to pravastatin plus primaquine 2mM. After 30 min, the erythrocytes were hemolysed by adding distilled water (1:1). Then the lysates were used for the following biochemical investigations.
Assessment of erythrocytes non-protein thiols status
Erythrocytes NPSH were determined using Ellman's reagent, 5, 5-dithiobis (2- nitrobenzoate). Protein was precipitated with adding 1:1 volume of 5% trichloroacetic acid (TCA). After centrifugation, the supernatant was neutralized with Tris-NaOH and NPSH were quantified in supernatant [17].
Assessment of erythrocytes protein oxidation
Protein oxidation erythrocytes were assayed as protein carbonyl according to the method of Levine et al. [18]. Proteins were precipitated from RBCs lysates by addition of 10% TCA and resuspended in 1.0 ml of 2 M HCl for blank and 2 M HCl containing 2% 2,4- dinitrophenyl hydrazine. After incubation for 1 h at 37°C, protein samples were washed with alcohol and ethyl acetate, and re-precipitated by addition of 10% TCA. The precipitated protein was dissolved in 6 M guanidine hydrochloride solution and measured at 370 nm. Calculations were made using the molar extinction coefficient of 22×103M−1 cm−1 and expressed as nmol carbonyls formed per mg protein. Total protein in RBC pellet was assayed according to the method of Lowry et al. [19] using bovine serum albumin as standard.
Assessment of erythrocytes lipids peroxidation
Thiobarbituric acid reactive substance (TBARS) was determined as indicator of lipid peroxidation in erythrocytes by a spectrophotometric method [20]. A mixture of 200 μL of 8% sodium dodecyl sulfate, 200 μL of 0.9% thiobarbituric acid and 1.5 ml 20% acetic acid was prepared. 200 μL of RBCs lysate and 1.9 ml distilled water were added to complete the volume of 4 ml. After boiling for 1 h, the mixture was cooled, and 5 ml of n-butanol and pyridine (15:1) solution was added to it. This mixture was then centrifuged at 5000 rpm for 15 min and the absorbance was measured at 532 nm. Quantification of MDA levels was performed using tetraethoxypropane as the standard.
Determination of erythrocytes hemolysis
Erythrocytes hemolysis was determined by osmotic fragility behavior using different NaCl solutions. A 25 μL of blood samples from all studied groups were added to a series of 2.5 ml saline solutions (0.0 to 0.9 % of NaCl). After gentle mixing and standing for 15 min at room temperature the erythrocytes suspensions were centrifuged at 1500 rpm for 5 min. The absorbance of released hemoglobin into the supernatant was measured at 540 nm [21].
Scanning electron microscopy (SEM)
Morphological differences between control and drug exposed erythrocytes was evaluated using JEOL JSM-6380 LA. Scanning electron microscope was used to evaluate the morphological differences between normal, pravastatin and primaquine exposed erythrocytes. All groups of erythrocytes were fixed in buffered gluteraldehyde. Aldehyde was drained and rinsed 3 times each of 5 min in phosphate buffer and post-fixed in osmium tetroxide for 1 h. After this, the samples were rinsed in distilled water and then dehydrated using a graded ethanol series; 25, 50, 75, 100 and another 100% each for 10 min. Then the samples were rinsed in water, removed, mounted on stabs, coated with gold and viewed under the SEM.
Statistical analysis
The statistical differences between groups were analyzed by one way ANOVA followed by TUKEY Kramer multiple comparison test, using GraphPad Prism Software v 5.01. The values at P < 0.05 were chosen as statistically significant.
Results
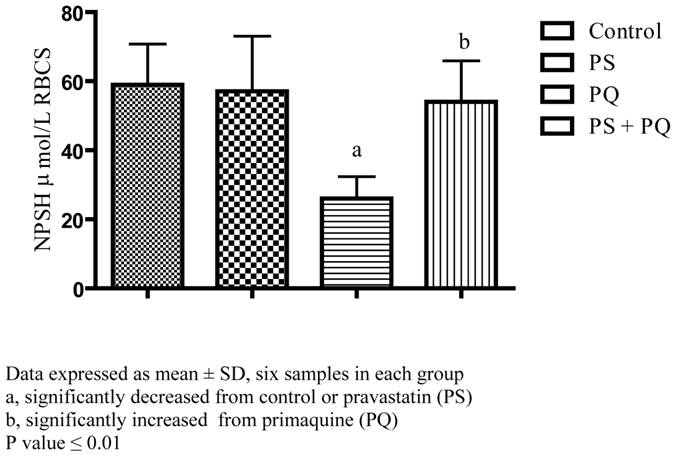
Our results revealed that incubation of erythrocytes for 30 min with pravastatin at concentration 2mM do not change the NPSH level in erythrocytes (57.13 ± 6.50) versus erythrocytes free drug (58.93 ± 4.81). While exposure of erythrocytes to 2 mM primaquine alone was resulted in a significant decrease of NPSH content (26.05 ± 2.58) compared with control erythrocytes as well as pravastatin exposed erythrocytes. Pretreatment of erythrocytes with 2mM of pravastatin before primaquine exposure preserve NPSH level (54.03 ± 4.84) regarding to RBCs incubated with PQ alone, Figure 1.
Effect of pravastatin and primaquine on erythrocytes non protein thiols (NPSH) level.
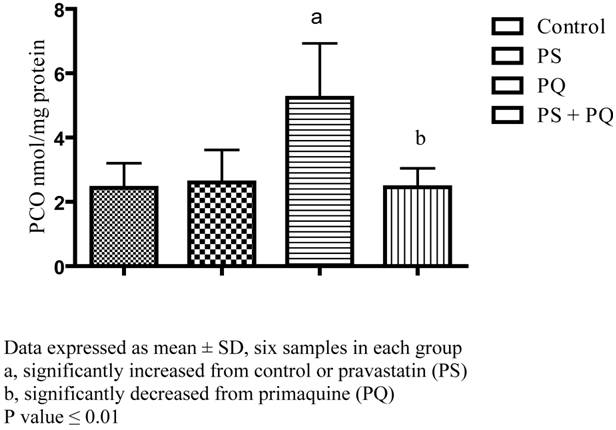
In this study, there is considerable elevation of PCO content of erythrocytes treated with 2mM of primaquine by about 115% in relation to either control erythrocytes or erythrocytes treated with pravastatin. On the other hand, erythrocytes treated with 2mM of pravastatin exert no change in PCO level in relation to control one. Moreover, prior incubation of erythrocytes with pravastatin keep away from primaquine induced elevation of PCO content by about 113%, see Figure 2.
Effect of pravastatin and primaquine on erythrocytes protein carbonyl level.
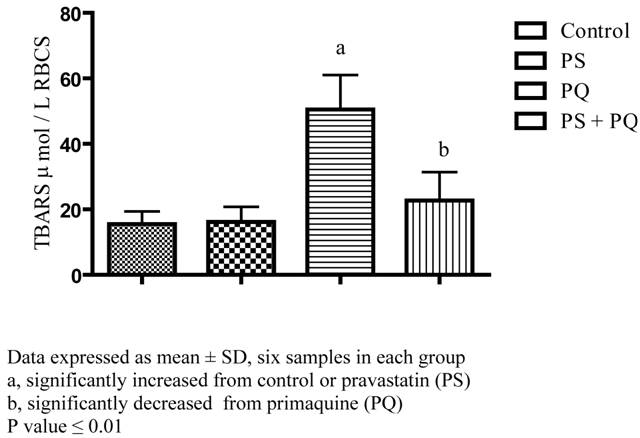
In respect to TBARS our results showed that incubation of erythrocytes with PQ exert significant elevation of TBARS by about 225% versus erythrocytes free drug as well as erythrocytes supplemented with pravastatin. Furthermore, pravastatin treatment at the same time with primaquine preserves the erythrocytes TBARS content at value near that of the control group see Figure 3.
Effect of pravastatin and primaquine on erythrocytes thiobarbituric acid reactive substance (TBARS) level.
Hemolysis profile of control erythrocytes and erythrocytes incubated with pravastatin, primaquine alone or in combination is revealed in Table 1. The results of this work demonstrated that, NaCl at 0-0.2% concentration range, there is no significant difference in the erythrocytes hemolysis in percent between primaquine, pravastatin as well as control erythrocytes. Conversely, NaCl at 0.3-0.9% concentration range, there is significant increase in the percent of RBCs hemolysis for primaquine in comparison with the other groups (P<0. 001).
Hemolysis profile of control erythrocytes and erythrocytes exposed to either PRV or PQ at concentration 2 m mole /L
| NaCl g/L | % of erythrocytes hemolysis | |||
|---|---|---|---|---|
| Control | PS | PQ | PS+ PQ | |
| 1.0 | 94.8 ± 9.24 | 98.4 ± 8.65 | 99.5 ± 8.03 | 95.2 ± 9.63 |
| 2.0 | 88.2 ± 8.70 | 89.2 ± 9.53 | 97.9 ± 6.05 | 90.2 ± 7.63 |
| 3.0 | 62.8 ± 14.3 | 63.2 ± 10.8 | 83.5 ± 12.5 *a | 64.4 ± 8.50 *b |
| 4.0 | 27.8 ± 5.16 | 31.3 ± 7.64 | 51.5 ± 13.3**a | 37.3 ± 6.43*b |
| 5.0 | 21.3 ± 7.50 | 22.3 ± 9.49 | 40.6 ± 8.71a | 23.8 ± 9.82 *b |
| 6.0 | 11.7 ± 3.39 | 12.9 ±3.28 | 27.4 ± 6.34 ***a | 14.2 ± 2.00***b |
| 7.0 | 5.18 ± 1.90 | 6.79 ±2.22 | 16.2 ± 3.61 ***a | 9.05 ± 2.00***b |
| 8.0 | 2.88± 1.78 | 2.51 ± 0.86 | 9.07 ± 2.60 ***a | 3.96±1.54 ***b |
| 9.0 | 1.28 ± 0.55 | 1.42± 1.01 | 2.76 ± 1.04 *a | 2.28 ±0.85 |
Data expressed as mean ± SD, six samples in each group
a, significantly increased from control or pravastatin (PS)
b, significantly decreased from primaquine (PQ)
*, P value ≤ 0.05
**, P value ≤ 0.01
***, P value ≤ 0.05
In this study, our data also show that the minimum hemolysis of erythrocytes (1.28%, 1.42%, 2.76 % and 2.28%) was observed at NaCl concentration of 0.9 % for control, pravastatin, primaquine and their combinations respectively. On another side the maximum hemolysis of 94.8% for control erythrocytes, 98.4% for pravastatin, 99.5% for primaquine and 95.2% for the combination between pravastatin and primaquine was occurred at NaCl concentration of 0.1%.
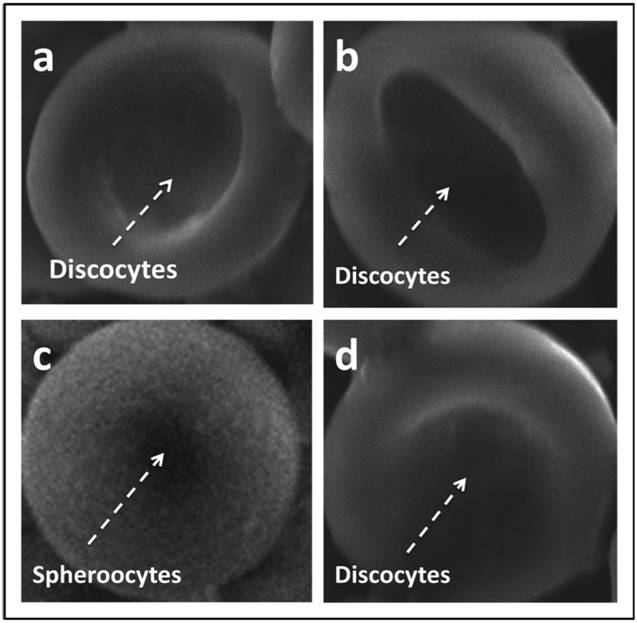
Typical micrographs of erythrocytes obtained following exposure to drugs has been depicted in Figure 4. Control erythrocytes and erythrocytes incubated (for 30 min) with pravastatin, primaquine, as well as their combinations at 2 mM concentrations were screened for any observable morphological alterations using scanning electron microscope (SEM). Our results showed the spherocytes formation as a result of primaquine incubation. But in control group, pravastatin as well as pravastatin plus primaquine treatment showed the normal discocyte shape of erythrocytes was preserved.
Scanning electron microscope graphing of (a) control RBC, (b) RBC incubated with 2 mM PS, (c) RBC exposed to 2 mM of PQ (d) RBCs exposed to same concentration of PS plus PQ. Note spherocytes formation on case of primaquine treatment(c). Magnification x5.500.
Discussion
Erythrocytes have been proposed as real-time biomarkers in many diseases. However, changes of RBCs have been detected in a number of human pathologic conditions or exposure to xenobiotics displaying oxidative stress. So that the preservation of erythrocytes functions is believable to protect against the development of many diseases. In this study we have investigated the protective effect of pravastatin against primaquine induced oxidative stress in human erythrocytes.
NPSH mostly GSH, cysteine, coenzyme A and other thiols play important role in cytoprotection against oxidative stress [22]. Therefore, the decrease of NPSH levels in erythrocytes, making them more susceptible to oxidative insult. Nonetheless, primaquine mediate oxidative stress through interaction with NADPH, as well as auto-oxidation leading to generation of ROS such as hydrogen peroxide, superoxide as well as hydroxide radicals [23]. The significant decrease of NPSH in erythrocytes after incubation with primaquine is due to interaction of ROS with NPSH oxidizing them. On the contrary, statins have ability to inhibit the production of ROS as well as maintains the antioxidants activity in the cell [24]. Moreover it has been reported that supplementation of antioxidants preserve the NPSH from oxidative damage [25]. Therefore, pravastatin can protect the erythrocytes NPSH against primaquine induced oxidation. These findings are in agreement with the previous study established that antioxidants supplementation preserve cellular thiols and maintains the cells integrity [26].
Oxidation of proteins can introduce carbonyl groups at some amino acids residues such as lysine, arginine, proline, and threonine in the polypeptide chains [27]. PCO level was assessed to evaluate primaquine-mediated protein oxidative damage. In our observation there is marked elevation of erythrocytes PCO level by primaquine exposure is noticed. These findings are in accordance with pervious study reported that in vitro exposure of RBCs to oxidants resulted in damaging of protein in addition to increase PCO formation [27]. This may suggest that oxidant drugs increase free radicals production in red blood cells and decrease the activities of antioxidant enzymes [26]. Furthermore, proteinases that protect erythrocytes proteins by degrading the oxidatively damaged proteins are lost during oxidative stress [28].
Pravastatin treatment protects the erythrocytes against primaquine induced protein oxidation. These results are with the same observation stated that pravastatin maintains catalase activity; however catalase is one of the important antioxidant enzymes in erythrocytes [29]. The reduction of NPSH by primaquine is a clear indication of oxidative stress, leading to protein oxidation as well as increase of erythrocytes TBARS as indicator for lipids peroxidation. Pravastatin inhibits the oxidative stress induced by primaquine through normalization of TBARS as well as PCO levels. However, statins protects against lipids peroxidation in different situation of oxidative stress [30]. Likewise, there are some reports which suggested that antioxidants are able to decrease the oxidative stress caused by drugs or chemicals [31].
Osmotic fragility is used to display structural changes of the RBC membrane when they are subjected to osmotic stress [32]. In the present study, the susceptibility of erythrocytes to hemolysis in presence of primaquine was greater than that of control in addition to pravastatin treated erythrocytes. This finding are similar to the previous study reported that exposure of antimalarial drugs to high iron level found in the RBCs create free radicals that are highly destructive to erythrocytes plasma membrane [32]. Furthermore, increase of protein oxidation in erythrocytes as well as a significant decrease in sulfhydryl content clearly indicate the presence of oxidative stress in erythrocytes membrane [33]. Increased oxidative stress may be responsible for the increased fragility of primaquine treated erythrocytes. Furthermore, free radicals can overwhelm the capacity of antioxidants enzymes to maintain and keep up the membrane integrity [34].
The major alteration in the shape of erythrocytes is the spherocytes formation in the presence of primaquine. These observations are supported by the work done by Prasanthi et al., in 2005 which reported that the shape changes of erythrocytes are induced by addition of some drugs. Spherocytes formation may be due to alteration of structural protein of the membrane as a result of protein oxidation [35].
Finally, it can be concluded that increased protein and lipid oxidation during PQ exposure destabilize the membrane of erythrocytes leading to significant increase of erythrocytes hemolysis. Pravastatin treatment can protect erythrocytes against primaquine induced oxidative damage due to antioxidant action. Furthermore, it is concluded that pravastatin can be used to preserve the erythrocytes functions during conditions associated with increased oxidative stress such as drug induced oxidative damage.
Acknowledgements
The author would like to thank Dr. Gamal Harisa, Kayyali Chair for Pharmaceutical Industry, College of Pharmacy, King Saud University for his assistance. Also, Dr. Omar Abdel-Kader, SEM Unit, Zoology Department, College of Science, King Saud University, for SEM analysis. This work was funded by Kayyali Chair for the Pharmaceutical Industry.
Conflict of Interest
The author(s) have declared that no conflict of interest exists.
References
1. Maurizio M, Luciano A, Walter M. The microenvironment can shift erythrocytes from a friendly to a harmful behavior: Pathogenetic implications for vascular diseases. Cardiovas Res. 2007;75:21-28
2. Çimen MYB. Free radical metabolism in human erythrocytes. Clinica Chimica Acta. 2008;390:1-11
3. Durak I, Kavutcu M, Çimen MYB, Elgün S, Öztürk H.S. Oxidant/ antioxidant status of erythrocytes from patients with chronic renal failure: effects of hemodialysis. Med Princ Pract. 2001;10:187-90
4. Asgary S, Naderi GH, Askari N. Protective effect of flavonoids against red blood cell hemolysis by free radicals. Exp Clin Cardiol. 2005;10(2):88-90
5. Grinberg LN, Rachmilewitz EA, Newmark H. Protective effects of rutin against hemoglobin oxidation. Biochem Pharmacol. 1994;48:643-649
6. Robaszkiewicz A, Bartosz G, Soszynski M. N-chloroamino acids cause oxidative protein modifications in the erythrocytes membrane. Mech Ageing Dev. 2008;129:572-529
7. Prasanthi K, Muralidhara, Rajini PS. Morphological and biochemical perturbations in rat erythrocytes following in vitro exposure to Fenvalerate and its metabolite. Toxicol In Vitro. 2005;19:449-456
8. Fraser IM, Vessel ES. Effects of metabolites of primaquine and acetanilide on normal and glucose-6- phosphate dehydrogenase-deficient erythrocytes. J Pharm Exp Ther. 1968;162:155-165
9. Thornally PJ, Stern A, Bannister JV. A mechanism for primaquine mediated oxidation of NADPH in red blood cells. Biochem Pharmacol. 1983;32:3571- 3575
10. Bowman ZS, Morrow JD, Jollow D J, McMillan D. C. Primaquine-Induced Hemolytic Anemia: Role of Membrane Lipid Peroxidation and Cytoskeletal Protein Alterations in the Hemotoxicity of 5-Hydroxyprimaquine. J Pharmacol Exp Ther. 2005;314:838-845
11. Sulekha M, Satish Y, Sunita Y, Rajesh KN. Antioxidants: A Review. J Chem and Pharmaceu Res. 2009;1:102-104
12. Wainwright CL. Statins: is there no end to their usefulness? Cardiovasc Res. 2005;65:296-298
13. Liao JK. Effect of statins on 3-hydroxy-3-methylglutaryl coenzyme A reductase inhibition beyond low-density lipoprotein cholesterol. Am J Cardiol. 2005;96:24F-33F
14. Li X, Liu C, Cui J, Dong M, Peng CH, Li QS, Cheng JL, Jiang SL, Tian Y. Effects of pravastatin on the function of dendritic cells in patients with coronary heart disease. Basic Clin Pharmacol Toxicol. 2009;104:101-106
15. Kassan M, Montero MJ, Sevilla MA. Chronic treatment with pravastatin prevents cardiovascular alterations produced at early hypertensive stage. Br J Pharmacol. 2009;158:541-547
16. Beutler E. Red Cell Metabolism. New York: Grune and Stratton Inc. 1971
17. Ellman GL. Tissue sulphydryl groups. Arch Biochem Biophys. 1959;82:70-77
18. Levine L, Williams J, Stadtman R, Shacter E. Carbonyl assay for determination of oxidatively modified proteins. Methods Enzymol. 1994;233:346-357
19. Lowery OH, Rosenbrough NJ, Randall RJ. Protein measurement with Folin phenol reagent. J Biol Chem. 1951;193:265-75
20. Ohkawa H, Ohisshi N, Yagi K. Assay of lipid peroxidation in animal tissues by thiobarbituric acid reaction. Anal Biochem. 1979;95:351-358
21. Kraus A, Roth HP, Kirchgessner M. Supplementation with Vitamin C, Vitamin E or b-carotene influences osmotic fragility and oxidative damage of erythrocytes of zinc-deficient rats. J Nutr. 1997;127:1290-1296
22. Lajos N, Miki N, Sandor S. Protein and non-protein sulfhydryls and disulfides in gastric mucosa and liver after gastrotoxic chemicals and sucralfate: Possible new targets of pharmacologic agents. World J Gastroenterol. 2007;13:2053-2060
23. Augusto O, Weingrill CLV, Schreier S, Amemiya H. Hydroxyl radical formation as a result of the interaction between primaquine and reduced pyridine nucleotides. Arch Biochim Biophys. 1986;244:147-155
24. Sanguigni V, Pignatelli P, Caccese D. Atorvastatin decreases platelet superoxide anion production in hypercholesterolemic patients. Eur Heart J. 2002;4:372
25. Carty JL, Bevan R, Waller H, Mistry N, Cooke M, Lunec J, Griffiths HR. The effects of vitamin C supplementation on protein oxidation in healthy volunteers. Biochem Biophys Res Com. 2000;273:729-735
26. Karabulut I, Balkanci ZD, Pehlivanoglu B, Erdem A, Fadillioglu E. Effect of toluene on erythrocytes membrane stability under in vivo and in vitro conditions with assessment of oxidant/antioxidant status. Toxicol Ind Health. 2009;25:545-50
27. Amici A, Levine RL, Tsai L, Stadtman ER. Conversion of amino acid residues in proteins and amino acid homopolymers to carbonyl derivatives by metal-catalyzed oxidation reactions. J Biol Chem. 1989;264:3341-3346
28. Beppu M, Inoue M, Ishikawa T, Kikugawa K. Presence of membrane-bound proteinases that preferentially degrade oxidatively damaged erythrocytes membrane proteins as secondary antioxidant defense. Biochim Biophys Acta. 1994;1196:81-87
29. Broncel M, Koter-Michalak M, Chojnowska-Jezierska J. The effect of statins on lipids peroxidation and activities of antioxidants enzymes in patients with dyslipidemia. Zegl Lek. 2006;63:738-742
30. Maria K, Ida F, Marlena B, Julita C. Effects of simvastatin and pravastatin on peroxidation of erythrocytes plasma membrane lipids in patients with type 2 hypercholesterolemia. Can J Physiol Pharmacol. 2003;81:485-492
31. Krukoski DW, Comar SR, Claro LM, Leonart MS, Nascimento AJ. Effect of vitamin C, deferoxamine, quercetin and rutin against tert-butyl hydroperoxides oxidative damage in human erythrocytes. Hematology. 2009;14:168-172
32. Okwusidi JI. Long term storage stabilizes human erythrocytes membrane in Nigerian black males. African J Biomed Res. 2004;7:9-12
33. Gul O, Selda K, Yusuf O, Gulcin A, Mujdat U. Lipid and protein oxidation in erythrocytes membranes of hypercholesterolemic subjects. Clin Biochem. 2001;34:335-339
34. Chikezie PC, Uwakwe AA Monago CC. Studies of human HbAA erythrocytes osmotic fragility index of non malarious blood in the presence of five antimalarial drugs. J Cell and Animal Biol. 2009;3:39-43
35. Michaels LA, Cohen AR, Zhao H, Raphael RI, Manno CS. Screening for hereditary spherocytosis by use of automated erythrocytes indexes. The Journal of pediatrics. 1997;130:957-960
Author contact
Corresponding author: Email: afarscom.

 Global reach, higher impact
Global reach, higher impact