Impact Factor ISSN: 1449-1907
Int J Med Sci 2009; 6(6):358-364. doi:10.7150/ijms.6.358 This issue Cite
Research Paper
980 nm diode lasers in oral and facial practice: current state of the science and art
1. Department of Dental Sciences and Surgery, University of Bari, Bari, Italy
2. Department of Internal Medicine, Immunology and Infectious Diseases, Unit of Dermatology, University of Bari, Italy
Received 2009-6-23; Accepted 2009-11-20; Published 2009-11-24
Abstract
Aim: To evaluate the safety and efficacy of a 980nm diode laser for the treatment of benign facial pigmented and vascular lesions, and in oral surgery.
Materials and Methods: 20 patients were treated with a 980 nm diode laser.
Oral surgery: 5 patients (5 upper and lower frenulectomy). Fluence levels were 5-15 J/cm2; pulse lengths were 20-60 ms; spot size was 1 mm.
Vascular lesions: 10 patients (5 small angiomas, 5 telangiectases). Fluences were 6-10 J/cm2; pulse lengths were 10-50 ms; spot size was 2 mm. In all cases the areas surrounding the lesions were cooled.
Pigmented lesions: 5 patients (5 keratoses). All the lesions were evaluated by dermatoscopy before the treatment. Fluence levels were 7-15 J/cm2; pulse lengths were 20-50 ms; spot size was 1 mm.
All the patients were followed at 1, 4 and 8 weeks after the procedure.
Results: Healing in oral surgery was within 10 days. The melanoses healed completely within four weeks. All the vascular lesions healed after 15 days without any residual scarring.
Conclusions: The end results for the use of the 980 nm diode laser in oral and facial surgery appears to be justified on the grounds of efficacy and safety of the device, and good degree of acceptance by the patients, without compromising their health and function.
Keywords: 980 nm Diode Laser, pigmented lesions, vascular lesions, frenulectomy.
1. Introduction
Benign facial lesions both pigmented (keratoses, melanoses) and vascular (angiomas, linear telangiectases) are very frequent, and affect many adults of either sex with fair complexions [1,2].
Keratoses are circumscribed scaly lesions, located in the epidermis and composed of a proliferation of pigmented keratinocytes. Yellow-brown in colour, they range from dark yellow to black and can be divided into:
- seborrheic keratoses, with internal horny pseudocysts
- actinic or senile keratoses that develop in areas exposed to the sun.
Melanosis or hyperchromias are circumscribed pigmented lesions, with extracellular melanin pigment. They can be epidermal, dermal or mixed. They range in colour from black in superficial melanoses to brown in deep melanoses.
Angiomas are small elevated lesions, telangiectases (0.1-1mm diameter) are capillary dilatations of the subpapillary plexus. Red or pink in colour, they have thin walls with endothelial cells and slight basal membrane. Angiomas may show parietal endothelial proliferation. For some pigmented lesions (seborrheic) etiology is unknown, while the other pigmented lesions and the vascular lesions are brought about by solar and artificial irradiation as well as genetic predisposition.
In the past, besides chemical sclerosis for large vascular angiectasias, these lesions were treated by a variety of methods including electrocoagulation, cryotherapy, acid chemical agents (Trichloroacetic acid) and depigmenting agents (Hydrochinone), and C02, Ruby, Argon Laser systems either focussed or combined with dermoabrasive scanners [1-3].
The results were often evident scarring or dyschromia due to the lack of selectivity of the device; Ruby and Argon lasers, despite having an excellent chromophoric specificity for melanin-hemoglobin, did not allow photothermolysis owing to inappropriate pulsing for the treatment of smaller structures that don't require pulse durations of hundreds of milliseconds [4]. With Argon lasers, moreover, recurrences were frequent [3].
In medical practice a current treatment is now considered to be photocoagulation by Laser or Lamps with intense incoherent light, at selective wavelengths for melanin-hemoglobin chromophores, and emitting optimal pulses and fluences, in accordance with the principle of selective photothermolysis [3,5].
To this end, different monochromatic coherent sources may be used:
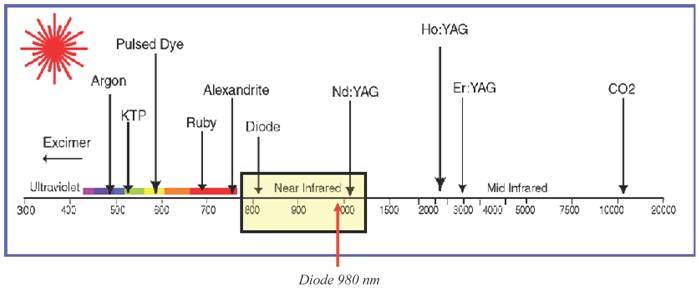
- in the visible region with: 1) green light 510, 532 nm, (Copper Br., KTP, Kripton); 2) yellow light 577, 585, 600 nm, (Dye, Vapour-Copper Br.); 3) red light 694 nm (Ruby)
- in the invisible region: - I.R. close to 755, 980, 1,064 nm (Alexandrite, Diode, Nd.-YAG). [Table 1]
Different lasers wavelength
The microcrusts resulting from vascular photosclerosis only last a few days and are to be considered a normal consequence of the treatment [6].
Only ultrashort pulses (450 ns) in a 577-600 nm Dye Lasers cause an unsightly purpora to develop on the vessels lasting 7-15 days as a result of the capillaries bursting under the excessively short shock waves [7]. This inconvenience delays the patients' return to their routine activities.
For the principle of selective photothermolysis to be respected Physics imposes a set of "ideal" theoretical parameters,which are:
- wavelength for selective absorption by chromophores: melanin (335-532 nm)[8], hemoglobinin(500-580nm;) [9,10], oxy-hemoglobin (580 nm;) [9,10], deoxy-hemoglobin(760nm;)[9,10]
- adequate fluence or energy dose;
- pulse duration proportionate to the target diameter to respect the thermal relaxation time.
When applying the technique in clinical practice operators should consider:
- the many individual cutaneous variables (phototype, scarring, site, chromia, size, thickness, depth of the lesion);
- the ability to control the equipment with critical assessment of the different Lasers and high-intensity Lamps in terms of size, weight, "fragility", learning curve and high equipment purchase and running costs.
The clinical evidence of lesions with inhomogeneous melanin distribution (yellow, brown and black tones) and oxydeoxyhemoglobin distribution (red, purple, blue) prompted us to question the efficacy of the 980nm Laser for photosclerosis of lesions and areas with little melanin and hemoglobin pigmentation [7].
Furthermore, to avoid exaggerated fluences and thermal damage to the surrounding tissues, and in accordance to J.A. Parrish's view [6] that exogenous chromophores are able to "target, manipulate, confine and control" the effects of Laser light in living system, in several cases is possible to use a readily available artificial photothermoabsorbant chromophore - 1% methylene blue - less expensive than the optimal indocyanine green, to mark the hypochromic keratoses and angiomas in order to artificially increase their ability to absorb the Laser light.
Innovative technologies such as the diode laser have provided considerable benefit to dental patients and professionals. Due to the conservative nature of treatment accomplished with the laser this technology is very useful in surgical dental procedures. The diode laser is utilized in both aesthetic enhancement of the smile, and treatment management of soft tissue issues [11].
Additionally Dental lasers contribute significantly to the field of cosmetic dentistry, providing an invaluable resource for clinicians who perform different types of aesthetic procedures. Practitioners in this specialized field not only help patients acquire beautiful and ideal smiles and dental health, but also they assist patients in benefiting from tremendous clinical advantages, such as bacterial reduction in surgical sites and increased comfort levels [11-18].
Following the suggestions of scientific literature on the advantages of the compactness, reliability, ease of use and affordability of the 980 nm Diode Lasers, we evaluated the efficacy and safety of one such Laser for the treatment of pathological frenulum, keratoses, angiomas and telangiectases.
2. PATIENTS AND METHODS
The treatment with the 980nm Diode Laser was proposed to a group of 15 patients phototypes 1-4, according to Fitzpatrick [19,20], with benign facial pigmented or vascular lesions, and to a group of 5 patients with pathological frenulum.
Exclusion criteria were a history of malignant pigment tumour, anticoagulation therapy or alterations in the clotting system and cutaneous wound healing with a tendency to form keloids.
Informed consent was obtained from all patients, in accordance with the declaration of Helsinki.
The diagnostic work-up included a clinical examination followed by videomicroscopy, to validate the preoperative diagnosis.
The lesions were also photographed before, immediately after and two months after treatment.
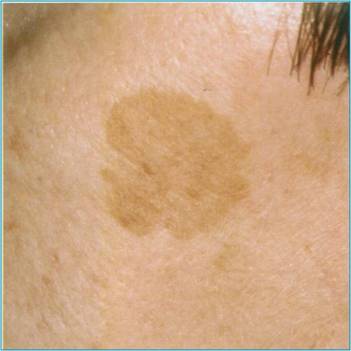
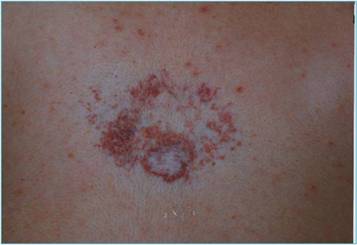
Pigmented lesions. This group comprised 5 patients (4 women and 1 men; age range 46-75 years); with senile keratosis (solar lentigo) [Fig.1a] varying in size from 2x2mm to 10xl5mm.
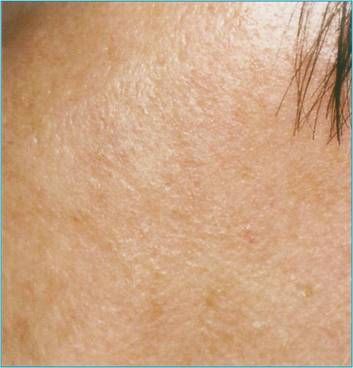
a: Solar lentigo cheek pretreatment. b: Solar lentigo 4 weeks after treatment
The area comprising the lesion was cooled by applying ice for 2 minutes immediately before and after the laser session.
The procedure was performed with fluences from 7 to 15 J/cm2, a pulse length of 20-50 ms, a spot diameter of 2 mm. In three "sensitive" patients we used a topical anaesthetic (EMLA® AstraZeneca LP, Wilmington, Del). A small anallergic plaster was applied for three days to the residual areas of the larger pigmentations.
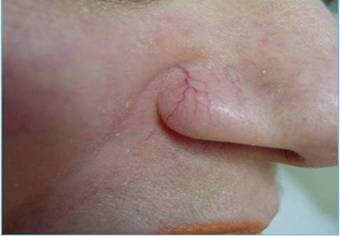
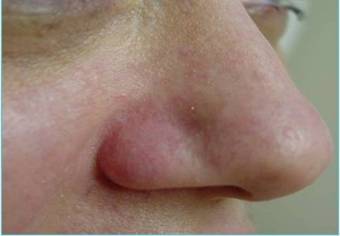
Vascular lesions. This group consisted of 10 patients (7 women and 3 men; age range 23-68 years). We treated 5 red linear telangiectases with diameters above 0.5mm [Fig.2a] and 5 angiomas ranging in size between 2x2 and 3x4 [Fig.3a]. All telangiectases were anaesthetised with cream (EMLA® AstraZeneca LP, Wilmington, Del) and then cooled by applying ice for 2 minutes before and after photosclerosis.
a: nasal telangiectases before treatment. b: nasal telangiectases 4 weeks after treatment
a: angioma pretreatment. b: angioma 4 weeks after treatment
The Laser settings were: fluence between 6 and 10 J/cm2, variable pulse length between 10 and 50 ms, and a spot diameter of 2 mm.
After the procedure the lesions were medicated for 5 days with a water-based cream containing 0.1% gentamicin and 0.1% betamethasone..
Oral surgery. This group comprised 5 patients. The Laser settings were: fluence between 5 and 15 J/cm2, variable pulse length between 20 and 60 ms, and a spot diameter less than 1mm in frenulectomy. Oral tissues were treated without local intra-tissue anaesthesia [17].
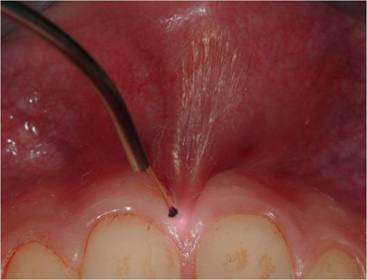
The patients described the procedure as totally painless [Fig.4a]. All patients returned to their routine activities without delay.
a: upper lip frenulum pretreatment. b: upper lip frenulum immediatedly post treatment. c: upper lip frenulum 10 days after treatment
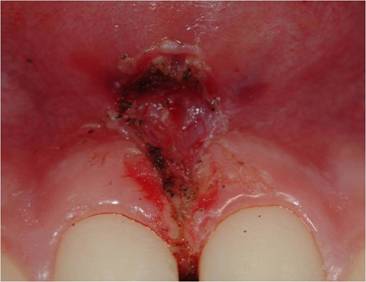
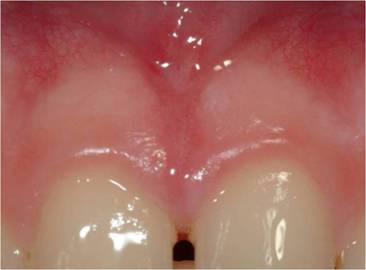
No haemorrhage was observed either during treatment or during the healing period.
All the patients were followed up at 1, 4, and 8 weeks from the procedure.
3. RESULTS
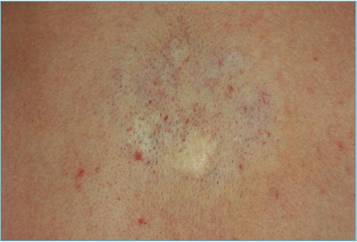
At the 4-week follow-up the cases of keratosis, had completely healed without scarring [Fig.1b]. There were no infections. All patients were satisfied with the treatment and the results obtained.
At the 4-week follow-up all the vascular lesions, had healed without leaving any macroscopically visible scars [Fig.2b,3b], after the appearance for half a day of erythema with moderate serum secretion and microcrasts for 5-7 days.
In all oral surgical procedures, no haemorrhage was observed either during treatment or during the healing period. No sutures were required. The patients were comfortable with no pain, either intra-operatively or post-operatively. Haemostasis was optimum immediately after the procedure [Fig.4b]. Ten days later the procedure, each healing was found to be uneventful [Fig.4c].
4. DISCUSSION AND CONCLUSIONS
Laser technology is developing very quickly. It is an instrument that achieves maximum oral health in a minimally invasive fashion. New Lasers with a wide range of characteristics are available today and are being used in the various fields of medicine and dentistry [4,7,9,12,20,21]. The search for new devices and technologies for dental procedures was always challenging and in the last two decades much experience and knowledge has been gained. Applications now are being developed for a broader range of wavelengths that will offer useful, predictable, and comfortable therapy for managing of dental patients. Particularly, the use of a diode laser seems to be promising, in patients, who need to be treated with a technique where the operative and post-operative blood loss and post-operative discomfort are reduced [17,18].
The lasers normally adopted offer the enormous advantage of being conveyed in a fibre, which serves as the working tip at the end of the handpiece. The use of flexible, length-adjustable optical fibre also enables efficacious irradiation i.e. the less accessible, deeper pockets in periodontal disease [13,15].
The most frequently used optical fibre has a diameter of 300 µm.
The targeted and controlled treatment of benign pigmented and vascular lesions using selective lasers (with wavelengths of 600-980 nm) and high-intensity lamps (Xenon) is now generally accepted. These are the most suitable tools for photocoagulating these small superficial lesions, allowing excellent results to be obtained painlessly, in a short time and without requiring the patients to suspend their routines activities.
For the operators, the main barriers to acquiring these tools are their high cost in terms of purchase, installation, management and, for some devices, even running and maintenance costs; space, weight and cooling devices that requires electrical systems to be upgraded are other factors that hinder the spread of these tools. In our practices we often encounter scars caused by naive operators who have been persuaded by unprofessional salespeople that "these intelligent machines" can replace "the brain and hand, skill and experience" of the specialist.
The aim of this study was to verify the reliability and efficacy of one of these compact portable diode instruments, emitting a maximum power density of 30W/cm2 not requiring pre-warming or controlling, and delivering a wavelength of 980 nm.
This device is naturally less selective and therefore less effective on melano-hemoglobin chromophores than those at less than 510-532-577 nm, which are however delivered by machines that:
- weigh up to over 100 Kg,
- are delicate as they can only be activated in air-conditioned environments with controlled temperatures,
- expensive in terms of maintenance and running costs.
Also Q-switched. Nd:YAG and ruby sources appear to be interesting [23-25].
Angiectases of the lower limbs, where the skin is thick, are deeper and are most often blue, and rarely purple-red. These lesions should all be treated after an accurate diagnosis and only after the major deep refluxes have been eliminated by surgery and sclerotherapy [26].
Purple-red angiectasias with a size of 1-3mm are arterial and/or arteriovenous and/or anteriovenous fistula dilatations; they are sometimes confused with neoangiogenesis or "matting", deriving from an "unfortunate" chemical sclerosis.
Although they have been described as venous capillary dilatations for their endothelial characteristics, they present greater oxygen saturation 76%, (69% for the blue ones) and have such a fast-flowing internal circulation that the scierotherapic substances are prevented from having sufficient contact to determine the reactive endothelitis and fibrosis.
In these cases lasers are indicated as a supplement to chemical sclerosis [26,27].
On the basis of the results obtained in the treatment of benign facial pigmented and vascular lesions, while recognising the physical limitations of the 980 nm wavelength compared to the absorption of more selective wavelengths, the use of a compact, portable 30 W Diode Laser appears to be justified as it has proved to be effective and safe and well-accepted by the patients.
The use of lasers in general dentistry is now an accepted and to some extent, expected treatment modality. Laser use can be either an adjunct to other procedures or the main form of treatment itself. For many procedures, lasers are now becoming the treatment of choice by both clinicians and patients, and in some cases, the standard of care. Clinicians need to learn more about constantly updated technology and apply newly discovered methods and protocols to clinical situations to benefit patients and clinicians.
Conflict of Interest
The authors have declared that no conflict of interest exists.
References
1. Tan T, Morelli J.G, Kurban A.K. Pulsed dye laser treatment of the benign cutaneous pigmented lesions. Laser Surg. Med. 1992;12:538
2. McCoy SE. Copper Bromide Laser Treatment of Facial Telangiectasia: Results of Patients Treated Over Five Years. Laser in Surg. Med. 1997;21:329-340
3. Anderson RR, Parrish JA. Selective photothermolysis: precise microsurgery by selective absorption of pulsed radiation. Science. 1983;220:524-527
4. Goldberg DJ. Laser Treatment of Vascular Lesions. Laser Dermatology. Berlin Heidelberg: Springer. 2005:13-35
5. van Gemert MJ, Welch AJ, Pickering JW, Tan OT, Gijsbers GH. Wavelengths for laser treatment of port wine stains and telangiectasia. Lasers Surg Med. 1995;16(2):147-55
6. Parrish JA. Afterword: A Look Ahead. Cutaneous Laser Surgery. St. Louis, Missouri: Mosby Inc. 1999:491-492
7. Anderson PR. Laser — Tissue Interactions. Cutaneous Laser Surgery. St. Louis, Missouri: Mosby Inc. 1999:13-18
8. Kollias N. The spectroscopy of human melanin pigmentation. Melanin: Its Role in Human Photoprotection. Valdenmar Publishing Co. 1995:31-38
9. Papel I.D. Laser in facial plastic surgery. Facial plastic and reconstructive surgery, 2nd Edition, pp 79-95. New York Thieme Medical Publisher Inc
10. Tseng SH, Bargo P, Durkin A, Kollias N. Chromophore concentrations, absorption and scattering properties of human skin in-vivo. Opt Express. 2009;17(17):14599-617
11. Reichwage DP, Barjenbruch T, Lemberg K, Janiszewski T, Marr D. Esthetic contemporary dentistry and soft tissue recontouring with the diode laser. J Indiana Dent Assoc. 2004;83(1):13-5
12. AdamsTC Pang PK. Lasers in aesthetic dentistry. Dental Clinics of North America. 2004;48(4):833-860
13. Romanos GE, Henze M, Banihashemi S, Parsanejad HR, Winckler J, Nentwig GH. Removal of epithelium in periodontal pockets following diode (980 nm) laser application in the animal model: an in vitro study. Photomed Laser Surg. 2004Jun;22(3):177-83
14. Capodiferro S, Maiorano E, Scarpelli F, Favia G. Fibrolipoma of the lip treated by diode laser surgery: a case report. J Med Case Reports. 2008;2:301
15. de Souza EB, Cai S, Simionato MR, Lage-Marques JL. High-power diode laser in the disinfection in depth of the root canal dentin. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2008;106:e68-72
16. Kafas P, Dabarakis N, Theodoridis M. Performing gingivoplasty without injected anaesthesia: a case report. Surg J. 2008;3:27-29
17. Kafas P, Angouridakis N, Dabarakis N, Jerjes W. Diode laser lingual frenectomy may be performed without local anaesthesia. Int J Orofac Sci. 2008;1:1
18. Sarver DM, Yanosky M. Principles of cosmetic dentistry in orthodontics: part 2. Soft tissue laser technology and cosmetic gingival contouring. Am J Orthod Dentofacial Orthop. 2005;127:85-90
19. Fitzpatrick TB. Dermatology 1945-95: the golden age of treatment. J Dermatol. 1996Nov;23(11):728-34
20. Fitzpatrick TB. The skin cancer cascade: from ozone depletion to melanoma--some definitions and some new interpretation, 1996. J Dermatol. 1996Nov;23(11):816-20
21. Antenucci EL. Integration of lasers into a soft tissue management program. Dent Clin North Am. 2000Oct;44(4):811-9
22. Coluzzi DJ, Goldstein AJ. Lasers in dentistry. An overview. Dent Today. 2004;23(4):120-7
23. Cassuto D.A, Ancona DM, Emanuelli G. Treatment of facial telangiectasias with a diode-pumped Nd:YAG laser at 532 nm. J Cutan Laser Ther. 2000;2(3):141-6
24. Goldberg DJ, Meine JG. Treatment of facial telangiectases with the diode-pumped frequency-doubled Q-switched Nd:YAG laser. Dermatol Surg. 1998Aug;24(8):828-32
25. Sadighha A, Saatee S, Muhaghegh-Zahed G. Efficacy and adverse effects of Q-switched ruby laser on solar lentigines: a prospective study of 91 patients with Fitzpatrick skin type II, III, and IV. Dermatol Surg. 2008Nov;34(11):1465-8
26. Dover JS, Sadick NS, Goldman MP. The role of laser and light sources in the treatment of leg veins. Dermatol. Surg. 1999;254:328-336
27. Dudelzak J, Hussain M, Goldberg DJ. Vascular-specific laser wavelength for the treatment of facial telangiectasias. J Drugs Dermatol. 2009Mar;8(3):227-9
Author contact
Correspondence to: Dr. Andrea BALLINI, PhD., Department of Dental Sciences and Surgery, University of Bari, Bari, Italy, Faculty of Medicine and Surgery, University of Bari, Piazza G. Cesare n.11, 70124 - Bari - Italy. Tel. (+39) 0805594242; Fax. (+39)0805478043; E-mail: andrea.balliniuniba.it

 Global reach, higher impact
Global reach, higher impact